Definition
Myopathies are diseases of skeletal muscle which are not caused by nerve disorders. These diseases cause the skeletal or voluntary muscles to become weak or wasted.
Description
There are many different types of myopathies, some of which are inherited, some inflammatory, and some caused by endocrine problems. Myopathies are rare and not usually fatal. Typically, effects are mild, largely causing muscle weakness and movement problems, and many are transitory. Only rarely will patients become dependent on a wheelchair. However, muscular dystrophy (which is technically a form of myopathy) is far more severe. Some types of this disease are fatal in early adulthood.
Causes & symptoms
Myopathies are usually degenerative, but they are sometimes caused by drug side effects, chemical poisoning, or a chronic disorder of the immune system.
Genetic myopathies
Among their many functions, genes are responsible for overseeing the production of proteins important in maintaining healthy cells. Muscle cells produce thousands of proteins. With each of the inherited myopathies, a genetic defect is linked to a lack of, or problem with, one of the proteins needed for normal muscle cell function.
There are several different kinds of myopathy caused by defective genes:
- Central core disease
- Centronuclear (myotubular) myopathy
- Myotonia congenita
- Nemaline myopathy
- Paramyotonia congenita
- Periodic paralysis (hypokalemic and hyperkalemic forms)
- Mitochondrial myopathies.
Most of these genetic myopathies are dominant, which means that a child needs to inherit only one copy of the defective gene from one parent in order to have the disease. The parent with the defective gene also has the disorder, and each of this parent's children has a 50% chance of also inheriting the disease. Male and female children are equally at risk.
However, one form of myotonia congenita and some forms of nemaline myopathy must be inherited from both parents, each of whom carry a recessive defective gene but who don't have symptoms of the disease. Each child of such parents has a 25% chance of inheriting both genes and showing signs of the disease, and a 50% chance of inheriting one defective gene from only one parent. If the child inherited just one defective gene, he or she would be a carrier but would not show signs of the disease.
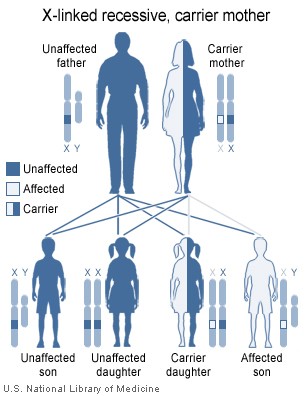
A few forms of centronuclear myopathy develop primarily in males. Females who inherit the defective gene are usually carriers without symptoms, like their mothers, but they can pass on the disease to their sons. Mitochondrial myopathies are inherited through the mother, since sperm don't contain mitochondria. (Mitochondria play a key role in energy production in the body's cells.)
The major symptoms associated with the genetic myopathies include:
- Central core disease: mild weakness of voluntary muscles, especially in the hips and legs; hip displacement; delays in reaching developmental motor milestones; problems with running, jumping, and climbing stairs develop in childhood
- Centronuclear myopathy: weakness of voluntary muscles including those on the face, arms, legs, and trunk; drooping upper eyelids; facial weakness; foot drop; affected muscles almost always lack reflexes
- Myotonia congenita: voluntary muscles of the arms, legs, and face are stiff or slow to relax after contracting (myotonia); stiffness triggered by fatigue, stress, cold, or long rest periods, such as a night's sleep; stiffness can be relieved by repeated movement of the affected muscles
- Nemaline myopathy: moderate weakness of voluntary muscles in the arms, legs, and trunk; mild weakness of facial muscles; delays in reaching developmental motor milestones; decreased or absent reflexes in affected muscles; long, narrow face; high-arched palate; jaw projects beyond upper part of the face
- Paramyotonia congenita: stiffness (myotonia) of voluntary muscles in the face, hands, and forearms; attacks spontaneous or triggered by cold temperatures; stiffness made worse by repeated movement; episodes of stiffness last longer than those seen in myotonia congenita
- Periodic paralysis: attacks of temporary muscle weakness (muscles work normally between attacks); in the hypokalemic (low calcium) form, attacks triggered by vigorous exercise, heavy meals (high in carbohydrates), insulin, stress, alcohol, infection, pregnancy; in the hyperkalemic (normal/high calcium) form, attacks triggered by vigorous exercise, stress, pregnancy, missing a meal, steroid drugs, high potassium intake
- Mitochondrial myopathies: symptoms vary quite widely with the form of the disease and may include progressive weakness of the eye muscles (ocular myopathy), weakness of the arms and legs, or multisystem problems primarily involving the brain and muscles.
Endocrine-related myopathies
In some cases, myopathies can be caused by a malfunctioning gland (or glands), which produces either too much or too little of the chemical messengers called hormones. Hormones are carried by the blood and one of their many functions is to regulate muscle activity. Problems in producing hormones can lead to muscle weakness.
Hyperthyroid myopathy and hypothyroid myopathy affect different muscles in different ways. Hyperthyroid myopathy occurs when the thyroid gland produces too much thyroxine, leading to muscle weakness, some muscle wasting in hips and shoulders, and, sometimes, problems with eye muscles. The hypothyroid type occurs when too little hormone is produced, leading to stiffness, cramps, and weakness of arm and leg muscles.
Inflammatory myopathies
Some myopathies are inflammatory, leading to inflamed, weakened muscles. Inflammation is a protective response of injured tissues characterized by redness, increased heat, swelling, and/or pain in the affected area. Examples of this type include polymyositis, dermatomyositis, and myositis ossificans.
Dermatomyositis is a disease of the connective tissue that also involves weak, tender, inflamed muscles. In fact, muscle tissue loss may be so severe that the person may be unable to walk. Skin inflammation is also present. The cause is unknown, but viral infection and antibiotics are associated with the condition. In some cases, dermatomyositis is associated with rheumatologic disease or cancer. Polymyositis involves inflammation of many muscles usually accompanied by deformity, swelling, sleeplessness, pain, sweating, and tension. It, too, may be associated with cancer. Myositis ossificans is a rare inherited disease in which muscle tissue is replaced by bone, beginning in childhood.
Muscular dystrophy
While considered to be a separate group of diseases, the muscular dystrophies also technically involve muscle wasting and can be described as myopathies. These relatively rare diseases appear during childhood and adolescence, and are caused by muscle destruction or degeneration. They are a group of genetic disorders caused by problems in the production of key proteins.
The forms of muscular dystrophy (MD) differ according to the way they are inherited, the age of onset, the muscles they affect, and how fast they progress. The most common type is Duchenne MD, affecting one or two in every 10,000 boys. Other types of MD include Becker's, myotonic dystrophy, limb-girdle MD, and facioscapulohumeral MD.
Diagnosis
Early diagnosis of myopathy is important so that the best possible care can be provided as soon as possible. An experienced physician can diagnose a myopathy by evaluating a person's medical history and by performing a thorough physical exam. Diagnostic tests can help differentiate between the different types of myopathy, as well as between myopathy and other neuromuscular disorders. If the doctor suspects a genetic myopathy, a thorough family history will also be taken.
Diagnostic tests the doctor may order include:
- Measurements of potassium in the blood
- Muscle biopsy
- Electromyogram (EMG).
Treatment
Treatment depends on the specific type of myopathy the person has:
- Periodic paralysis: medication and dietary changes
- Hyperthyroid or hypothyroid myopathy: treatment of the underlying thyroid abnormality
- Myositis ossificans: medication may prevent abnormal bone formation, but there is no cure following onset
- Central core disease: no treatment
- Nemaline myopathy: no treatment
- Centronuclear (myotubular) myopathy: no treatment
- Paramyotonia congenita: treatment often unnecessary
- Myotonia congenita: drug treatment (if necessary), but drugs don't affect the underlying disease, and attacks may still occur.
Prognosis
The prognosis for patients with myopathy depends on the type and severity of the individual disease. In most cases, the myopathy can be successfully treated and the patient returned to normal life.
Muscular dystrophy, however, is generally a much more serious condition. Duchenne's MD is usually fatal by the late teens; Becker's MD is less serious and may not be fatal until the 50s.
Key Terms
- Electromyogram (EMG)
- A diagnostic test that records the electrical activity of muscles. In the test, small electrodes are placed on or in the skin; the patterns of electrical activity are projected on a screen or over a loudspeaker. This procedure is used to test for muscle disorders, including muscular dystrophy.
- Inflammation
- A protective response of injured tissues characterized by redness, increased heat, swelling, and/or pain in the affected area.
- Voluntary muscles
- Muscles producing voluntary movement.
Further Reading
For Your Information
Books
- Knowles, Anne. Under the Shadow. New York: Harper & Row, 1983.
Organizations
- Muscular Dystrophy Association. 3300 East Sunrise Dr., Tucson, AZ 85718. (520) 529-2000.
- National Arthritis and Musculoskeletal and Skin Diseases Information Clearinghouse. PO Box AMS, 9000 Rockville Pike, Bethesda, MD 20892. (301) 495-4484.
Other
- Facts About Myopathies. Tucson, AZ: Muscular Dystrophy Association, 1993.
Gale Encyclopedia of Medicine. Gale Research, 1999.