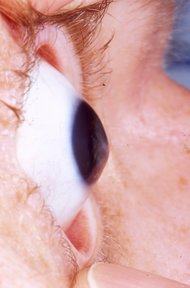
A structured approach to treating and billing.
Optometrists are often the first to see keratoconic patients, and we're the best qualified to serve their primary eyecare needs. We can fit them with glasses or contact lenses, or refer them for surgery.
Although many of us are fully capable of managing this condition, a lot of us are frustrated by the resistance of insurance companies to reimbursing us for our services. This article highlights a structured approach to managing and billing for keratoconus, which will benefit both you and your patients.
Keratoconus protocol
The following is my plan of action for keratoconic patients.
* Routine initial full exam for established patients (use code 92014) and new patients (use code 92004). Perform a full comprehensive eye exam. Document such things as corneal thinning, corneal striae, distorted mires, irregular astigmatism, scissors motion on retinoscopy as well as patient complaints about decreased vision, monocular diplopia and photophobia.
If you suspect keratoconus, bring your patient back for an evaluation. I tend not to perform corneal topography along with a full exam because by the time I confirm my suspicion of keratoconus, I've already performed applanation tonometry, which might distort the cornea.
Also, if the patient is a contact lens wearer and you postpone topography, have him discontinue lens wear to minimize corneal distortion. Plus, some insurances won't cover topography if it's performed at the time of the comprehensive exam.
* Intermediate exam (use code 92012) and corneal topo& raphy (use code 92499). Conduct an indepth history. Look for any family history of keratoconus or any of the associated factors, such as connective tissue disorders, Down's or Turner syndrome or any atopic conditions. Repeat keratometry, slit lamp examination and retinoscopy.
Now perform corneal topography. Even if you did so at the initial full exam, repeat here to verify results, especially if the patient is a contact lens wearer. Have him remove his lenses before this visit for as long as possible. If he needs them to see, schedule this appointment on a Monday, so he can wear his glasses on the weekend before the appointment.
If, by the end of this exam, you've confirmed your initial diagnosis of keratoconus, discuss options such as glasses, contact lenses and even corneal transplants with the patient. Typically, you'll proceed with a lens fitting after this visit.
At this point, send the patient's medical insurance company a letter of medical necessity for the contact lens fitting. Include enough detail to support your diagnosis and your reasoning for a contact lens fit. The letter shown on page 82 works well for me. I also enclose a copy of the topography.
During this intermediate visit, have the patient fill out a noncovered release form stating that he's responsible for the bill if the insurance doesn't cover it. If the patient is unsure of his medical coverage, have your office insurance person or the patient get pre-authorization before proceeding with the contact lens fit.
* Keratoconus contact lens fitting (see codes in letter on page 82). Include all contact lens checks in your contact lens fitting fee. Depending on the severity of the condition, estimate anywhere from three to five visits to finetune his prescription.
Your contact lens materials fee should cover the most expensive lenses you fit - generally the specialty RGP lenses. Even if you choose to fit a less expensive lens, it's wise to have one standard price for keratoconus lenses. Plus, you'll probably be billing an insurance company and will want uniform pricing.
It's often best to start with a high Dk value to permit adequate oxygen delivery to the cornea. I also advise the patient to initiate some sort of enzyming routine so the lenses stay free of deposits for longer.
* Follow-up (92012). After you finish the lens fitting process, see the patient after 1 month to assess his cornea. Check for staining with fluorescein dye and rose bengal.
If no corneal complications are present and the patient is happy with his lenses, check on him every 6 months. Repeat topography every year for mild or early keratoconus, and every 6 months for advanced stages.
The role of contact lenses
Managing keratoconus isn't limited to fitting contact lenses. In addition to regularly scheduled topography to monitor corneal changes, intermediate exams monitor the progression of the disease as well. This mode of treatment can add substantial income to your practice while you help your patients manage this condition.
In many cases, a patient's medical insurance will cover keratoconus contact lens fitting if you send the letter of medical necessity or call for pre-authorization. If it won't, don't prejudge your patient's willingness to pay for it. He'll accept a contact lens fit for keratoconus if you successfully convey the value he'll get. Plus, he'll be grateful for your help in managing his condition.
Not every keratoconic patient will require a contact lens fitting. In fact, I don't always rush early keratoconic patients into RGP lenses because of the long adaptation period. The vision for a patient should be decreased to 20/40 or 20/50 and improvable with RGPs. If a patient knows he'll get better vision with the lenses, he'll be more willing to put up with the initial adaptation period. If a patient hasn't been fit with RGPs and there's no significant corneal scarring, we have a pretty good idea of how much we can improve his vision.
In my practice, I find that roughly one-third of keratoconic patients are against RGPs. A handful opt for soft lenses, and the rest make do with what vision they get from their glasses.
In either case, these patients are valuable to my practice. Because I'm following these patients for a medical condition, they tend to be more loyal to my practice. In terms of dollar amount, I find that each keratoconic patient I have the satisfaction of helping in turn provides about $250 of additional revenue to my practice. And that's not even counting the contact lens fitting portion, which is about another $800.
Added value
Remember, you're the expert in this field, so patients are going to be more open to treatment options. After all, if their best corrected vision with eyeglasses is 20/80 and you get them to 20/30 with contact lenses, they'll be much happier with their lives, more productive at work and they'll feel much safer while driving.
If patients are willing to pay $4,000 for refractive sur-gery, then why wouldn't they pay $1,150 to enable them to see better than before?
Dr. Gupta works for Stam
ford Ophthalmology in Conn. He has no financial interest in any of the products or companies mentioned in
the article. You can reach Dr. Gupta at deegup4919@hotmail.com.
Copyright Boucher Communications, Inc. Jun 2001
Provided by ProQuest Information and Learning Company. All rights Reserved