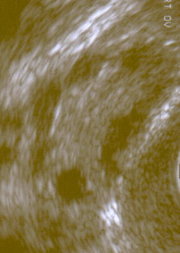
Definition
Polycystic ovary syndrome (PCOS) is a condition characterized by the accumulation of numerous cysts (fluid-filled sacs) on the ovaries associated with high male hormone levels, chronic anovulation (absent ovulation), and other metabolic disturbances. Classic symptoms include excess facial and body hair, acne, obesity, irregular menstrual cycles, and infertility.
Description
PCOS, also called Stein-Leventhal syndrome, is a group of symptoms caused by underlying hormonal and metabolic disturbances that affects about 6% of premenopausal women. PCOS symptoms appear as early as adolescence in the form of amenorrhea (missed periods), obesity, and hirsutism, the abnormal growth of body hair.
A disturbance in normal hormonal signals prevents ovulation in women with PCOS. Throughout the cycle, estrogen levels remain steady, LH levels are high, and FSH and progesterone levels are low. Since eggs are rarely or never released from their follicles, multiple ovarian cysts develop over time.
One of the most important characteristics of PCOS is hyperandrogenism, the excessive production of male hormones (androgens), particularly testosterone, by the ovaries. This accounts for the male hair-growth patterns and acne in women with PCOS. Hyperandrogenism has been linked with insulin resistance, the inability of the body to respond to insulin, and hyperinsulinemia (high blood insulin levels), both of which are common in PCOS.
Causes & symptoms
While the exact cause of PCOS is unknown, it runs in families, so the tendency to develop the syndrome may be inherited. The interaction of hyperinsulinemia and hyperandrogenism is believed to play a role in chronic anovulation in susceptible women.
The numbers and types of PCOS symptoms that appear vary between women. These include:
- Hirsutism. Related to hyperandrogenism, this occurs in 70% of women.
- Obesity. Approximately 40-70% of PCOS patients are overweight.
- Anovulation and menstrual disturbances. Anovulation appears as amenorrhea in 50% of patients, and as heavy uterine bleeding in 30% of patients; however, 20% of PCOS patients menstruate normally.
- Male-pattern hair loss. Some PCOS patients develop bald spots.
- Infertility. Achieving pregnancy is difficult in many women with PCOS.
- Polycystic ovaries. Most, but not all, women with PCOS have multiple cysts on their ovaries.
- Skin discoloration. Some women with PCOS have dark patches on the skin.
- Abnormal blood chemistry. Women with PCOS have high levels of low-density lipoprotein (LDL or "bad") cholesterol and triglycerides, and low levels of high-density lipoprotein (HDL or "good") cholesterol.
- Hyperinsulinemia. Some women with PCOS have high blood insulin levels, particularly if overweight.
Diagnosis
PCOS is diagnosed when the patient visits her doctor for treatment of symptoms such as hirsutism, obesity, menstrual irregularities, or infertility. PCOS patients are treated by a gynecologist, a doctor who treats diseases of the female reproductive organs, or a reproductive endocrinologist, a specialist who treats diseases of the body's endocrine (hormones and glands) system and infertility.
PCOS can be difficult to diagnose since its symptoms are similar to those of other diseases, and since all of its symptoms may not occur. The doctor takes a complete medical history, including questions about menstruation and reproduction, and weight gain. Physical examination includes a pelvic examination to determine the size of the ovaries, and visual inspection of the skin for hirsutism, acne, or other changes. Blood tests are performed to measure levels of LH, FSH, estrogens, androgens, glucose, and insulin. A glucose-tolerance test may be administered. An ultrasound examination of the ovaries is performed to evaluate their size and shape. Most insurance plans cover the costs of diagnosing and treating PCOS and its related problems.
Treatment
PCOS treatment is aimed at correcting anovulation, restoring normal menstrual periods, improving fertility, eliminating hirsutism and acne, and preventing future complications related to high insulin and blood lipid (fat) levels. Treatment consists of weight loss, drugs or surgery, and hair removal, depending upon which symptoms are most bothersome, and whether the patient desires pregnancy.
Weight loss
In overweight women, weight loss (as little as 5%) through diet and exercise may correct hyperandrogenism, and restore ovulation and fertility. This is often tried first.
Drugs
Hormonal drugs
Patients who do not want to become pregnant and require contraception (spontaneous ovulation occurs occasionally in PCOS patients) are treated with low-dose oral contraceptive pills (OCPs). OCPs bring on regular menstrual periods and correct heavy uterine bleeding, as well as hirsutism, although improvement may not be seen for up to a year.
If an infertile patient desires pregnancy, the first drug usually given to help induce ovulation is clomiphene citrate (Clomid), which results in pregnancy in about 70% of patients but can cause multiple births. In the 20-25% of women who do not respond to Clomid, other drugs that stimulate follicle development and induce ovulation, such as human menstrual gonadotropin (Pergonal) and human chorionic gonadotropin (HCG), are given; however, these drugs have a lower pregnancy rate (less than 30%), a higher rate of multiple pregnancy (from 5-30%, depending on the dose of the drug), and a higher risk of medical problems. PCOS patients have a high rate of miscarriage (30%), and may be treated with the gonadotropin-releasing hormone agonist leuprolide (Lupron) to reduce this risk.
Since PCOS patients do not have regular endometrial shedding due to high estrogen levels, they are at increased risk for overgrowth of this tissue and endometrial cancer. The drug medroxyprogesterone acetate, when taken for the first 10 days of each month, causes regular shedding of the endometrium, and reduces the risk of cancer. However, in most cases, oral contraceptive pills are used instead to bring about regular menstruation.
Other drugs
Another drug that helps to trigger ovulation is the steroid hormone dexamethasone. This drug acts by reducing the production of androgens by the adrenal glands.
The antiandrogen spironolactone (Aldactazide), which is usually given with an oral contraceptive, improves hirsutism and male-pattern baldness by reducing androgen production, but has no effect on fertility. The drug causes abnormal uterine bleeding and is linked with birth defects if taken during pregnancy. Another antiandrogen used to treat hirsutism, flutamide (Eulexin), can cause liver abnormalities, fatigue, mood swings, and loss of sexual desire. A drug used to reduce insulin levels, metformin (Glucophage), has shown promising results in PCOS patients with hirsutism, but its effects on infertility and other PCOS symptoms are unknown. Drug treatment of hirsutism is long-term, and improvement may not be seen for up to a year or longer.
Acne is treated with antibiotics, antiandrogens, and other drugs such as retinoic acids (vitamin A compounds).
Surgical treatment
Surgical treatment of PCOS may be performed if drug treatment fails, but it is not common. A wedge resection, the surgical removal of part of the ovary and cysts through a laparoscope (an instrument inserted into the pelvis through a small incision), or an abdominal incision, reduces androgen production and restores ovulation. Although laparoscopic surgery is less likely to cause scar tissue formation than abdominal surgery, both are associated with the potential for scarring that may require additional surgery. Laparoscopic ovarian drilling is another type of laparoscopic surgery used to treat PCOS. The ovarian cysts are penetrated with a laser beam and some of the fluid is drained off. From 50-65% of patients may become pregnant after either type of surgery.
Some cases of severe hirsutism are treated by hysterectomy and removal of the ovaries, followed by estrogen replacement therapy.
Other treatment
Hirsutism may be treated by hair removal techniques such as shaving, depilatories (chemicals that break down the structure of the hair), tweezing, waxing, electrolysis (destruction of the hair root by an electrical current), or the destruction of hair follicles by laser therapy; however, the treatments may have to be repeated.
Alternative treatments
PCOS can be addressed using many types of alternative treatment. The rebalancing of hormones is a primary focus of all these therapies. Acupuncture works on the body's energy flow according to the meridian system. Chinese herbs, such as gui zhi fu ling wan, can be effective. In naturopathic medicine, treatment focuses on helping the liver function more optimally in the horomonal balancing process. Dietary changes, including reducing animal products and fats, while increasing foods that nourish the liver such as carrots, dark green vegetables, lemons, and beets, can be beneficial. Essential fatty acids, including flax oil, evening primrose oil (Oenothera biennis), and black currant oil, act as anti-inflammatories and hormonal regulators. Western herbal medicine uses phytoestrogen and phytoprogesteronic herbs, such as blue cohosh (Caulophyllum thalictroides) and false unicorn root (Chamaelirium luteum), as well as liver herbs, like dandelion (Taraxacum mongolicum), to work toward hormonal balance. Supplementation with antioxidants, including zinc, and vitamins A, E, and C, is also recommended. Constitutional homeopathy can bring about a deep level of healing with the correct remedies.
Prognosis
With proper diagnosis and treatment, most PCOS symptoms can be adequately controlled or eliminated. Infertility can be corrected and pregnancy achieved in most patients although, in some, the hormonal disturbances and anovulation may recur. Patients should be monitored for endometrial cancer. Because of the high rate of hyperinsulinemia seen in PCOS, women with the disorder should have their glucose levels checked regularly to watch for the development of diabetes. Blood pressure and cholesterol screening are also needed because these women also tend to have high levels of LDL cholesterol and triglycerides, which put them at risk for developing heart disease.
Prevention
There is no known way to prevent PCOS, but if diagnosed and treated early, risks for complications such as and heart disease and diabetes may be minimized. Weight control through diet and exercise stabilizes hormones and lowers insulin levels.
Key Terms
- Androgens
- Male sex hormones produced by the adrenal glands and testes, the male sex glands.
- Anovulation
- The absence of ovulation.
- Antiandrogens
- Drugs that inhibit androgen production.
- Estrogens
- Hormones produced by the ovaries, the female sex glands.
- Hirsutism
- The abnormal growth of hair on the face and other parts of the body caused by an excess of androgens.
- Hyperandrogenism
- The excessive secretion of androgens.
- Hyperinsulinemia
- High blood insulin levels.
- Insulin resistance
- An inability to respond to insulin, a hormone produced by the pancreas that helps the body to use glucose.
- Ovarian follicles
- Structures found within the ovary that produce eggs.
Further Reading
For Your Information
Books
- Goldfarb, Herbert A., Zoe Graves, and Judith Greif. "Anovulation." In Overcoming Infertility: 12 Couples Share Their Success Stories. New York: John Wiley & Sons, 1995.
- Goldfarb, Herbert A., Zoe Graves, and Judith Greif. "Polycystic Ovary Disease (Stein-Leventhal Syndrome)." In Overcoming Infertility: 12 Couples Share Their Success Stories. New York: John Wiley & Sons, 1995.
- Kaptchuk, Ted J., Z'ev Rosenberg, and K'an Herb Co., Inc. K'an Herbals: Formulas by Ted Kaptchuk, O.M.D. San Francisco, CA: Andrew Miller, 1996.
- MacKay, H. Trent. "Gynecology: Persistent Anovulation (Polycystic Ovary Syndrome, Stein-Leventhal Syndrome)." In Current Medical Diagnosis and Treatment, edited by Lawrence M. Tierney, Jr., et al. Stamford, CT: Appleton & Lange, 1996.
- "Ovary Problems." In The Medical Advisor: The Complete Guide to Alternative & Conventional Treatments, edited by the editors of Time-Life Books. Alexandria, VA: Time-Warner, 1996.
- Speroff, Leon, Robert H. Glass, and Nathan G. Kase. "Anovulation and the Polycystic Ovary." In Clinical Gynecologic Endocrinology & Infertility, edited by Charles Mitchell. Baltimore, MD: Williams & Wilkins, 1994.
Periodicals
- "Excess Hair." Harvard Women's Health Watch (September 1997): 4-5.
- Franks, Stephen. "Polycystic Ovary Syndrome." New England Journal of Medicine 28 (September 1995): 853-861.
- Nestler John E., and Daniela J. Jakubowicz. "Decreases in Ovarian Cytochrome P450-17 Activity and Serum Free Testosterone After Reduction of Insulin Secretion in Polycystic Ovary Syndrome." New England Journal of Medicine 29 (August 1996): 617-623.
- Perlmutter, Cathy, and Maureen Sangiorgio. "Missing Periods." Prevention Magazine (October 1994): 81-83,134.
- "Polycystic Ovaries and Heart Disease." Harvard Women's Health Watch (September 1995): 7.
- "Polycystic Ovary Syndrome." Harvard Women's Health Watch (November 1996): 2-3.
Organizations
- American Academy of Dermatology. 930 N. Meacham Rd., Shaumburg, IL 60173-6016. (847) 330-0230. http://www.aad.org
- American College of Obstetricians and Gynecologists. 409 12th Street, SW, Washington, DC, 20024. (202) 638-5577. http://www.acog.org
- American Society for Reproductive Medicine. 1209 Montgomery Highway, Birmingham, AL 35216-2809. (205) 978-5000. http://www.asrm.com
- RESOLVE, Inc., 1310 Broadway, Somerville, MA 02144. (617) 623-0744. http://www.resolve.org
Gale Encyclopedia of Medicine. Gale Research, 1999.