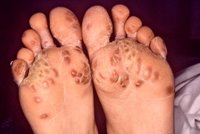
A 42 year-old African American female came to the emergency room complaining of fever, chills, and generalized pain in her joints, abdomen, and pelvis. Her symptoms began gradually over the previous 48 to 72 hours. She reported she had not been sexually active in the previous 3 weeks, and had no abnormal vaginal discharge, pharyngitis, or eye pain. She had only taken occasional acetaminophen and denied illicit drug use.
The physical exam revealed a temperature of 102.6[degrees]F orally but otherwise normal vital signs. Bilateral nonpurulent conjunctival infection (Figure 1) and oral mucosal inflammation (Figure 2) were plainly evident. Neck, chest, and cardiovascular examinations yielded no abnormal findings; however, her abdomen was diffusely tender without distension or organomegaly.
[FIGURES 1-2 OMITTED]
Pelvic exam revealed normal mucosa with thin white cervical discharge and cervical motion tenderness. Exam of the extremities showed no joint effusions or induration, but arthralgia was noted in both of her elbows, knees, and wrists. She had no rashes.
* WHAT IS THE DIFFERENTIAL DIAGNOSIS?
* WHAT ADDITIONAL TESTS SHOULD BE PERFORMED?
* WHAT IS THE INITIAL TREATMENT?
* DIFFERENTIAL DIAGNOSIS
This patient's symptoms included pelvic inflammatory disease, conjunctivitis, mucositis, and arthralgias. Diagnoses that would tie these signs and symptoms together include disseminated gonococcemia, chlamydial infections, Reiter's syndrome, and Stevens Johnson syndrome.
Lab tests: White blood cell count, chlamydia and other STDs
Her complete blood count revealed leukocytosis with a white blood cell count of 17,000 and a left shift of 6% bands. Endocervical DNA probe was positive for Chlamydia trachomatis. Blood cultures were negative.
Because many sexually transmitted diseases occur concurrently or are transmitted together, the patient was also tested for HIK, syphilis, and hepatitis B and C. The patient gave her consent for the HIV test, which came back negative. Serologies for syphilis and hepatitis B and C were drawn and found to be negative. A test for the human leukocyte antigen HLA-B27 was ordered because of the concern that this was Reiter's syndrome; the test result was negative.
* DIAGNOSIS: REITER'S SYNDROME
This patient was diagnosed with Reiter's syndrome, based on her clinical syndrome of conjunctivitis, arthralgias, mucositis, and cervicitis. The widespread distribution of the symptoms in this syndrome may be due to activation of the immune system by a viral or bacterial agent. (6,7)
The fact that her HLA-B27 test result was negative did not change this diagnosis; only 85% of patients with the syndrome are positive for HLA-B27, and the test results are frequently negative in African Americans. (4,5)
* INITIAL TREATMENT: ANTIBIOTICS AND ANTI-INFLAMMATORY AGENTS
The patient was hospitalized and started on intravenous ampicillin/sulbactam and oral azithromycin to cover for disseminated gonococcemia and chlamydia. Nonsteroidal anti-inflammatory medications were given for pain control. The patient rapidly responded to therapy as evidenced by decreased arthralgias, normalization of temperatures and white blood cell count, and decreased abdominal pain. The patient was discharged after the third day in the hospital with instructions to take doxycycline twice daily (finishing a 14-day course).
A positive DNA probe test for C trachomatis was helpful to guide therapy. As the availability of immunohistochemistry and polymerase chain reaction testing becomes more widely available, the number of cases of Reiter's syndrome without a documented infectious cause will likely diminish. (8)
DRUG BRAND NAMES
Ampicillin/sulbactam * Unasyn
Azithromycin * Zithromax
Doxycycline * Doryx, Monodox, Pefiostat, Vibramycin
REFERENCES
(1.) Centers for Disease Control and Prevention. STD Prevention. Chlamydia in the United States. April 2001. Available at www.cdc.gov/nchstp/dstd/Fact_Sheets/ chlamydia_facts.htm. Accessed on January 6, 2004.
(2.) Schneider JM, Matthews JH, Graham BS. Reiter's syndrome. Cutis 2003; 71:198-200.
(3.) Scoggins T. Reiter's syndrome. Available at: Emedicine.com. Accessed on January 4, 2004.
(4.) Fauci AS, Braunwald E, Isselbacher KJ, et al, eds. Harrison's Principles of Internal Medicine, Companion Handbook. 14th ed. New York, NY: McGraw-Hill; 1998:905-906.
(5.) Schumacher R, Klippel JH, Koopman WJ, et al, eds. Primer on the Rheumatic Diseases. 10th ed. Atlanta, Ga: Arthritis Foundation; 1993:160-161.
(6.) Parker CT, Thomas D. Reiter's syndrome and reactive arthritis. J Am Osteopath Assoc 2000; 100:101-104.
(7.) Prostatitis Foundation website. Reiter's syndrome briefing. 2003. Available at: http://www.prostatitis.org/reiters.html. Accessed on January 6, 2004.
(8.) Rahman MU, Cheema MA, Schumacher HR, Hudson AP. Molecular evidence for the presence of chlamydia in the synovium of patients with Reiter's syndrome. Arthritis Rheum 1992; 35:521-529.
Chlamydia trachomatis and Reiter's syndrome
An estimated 3 to 4 million cases of C trachomatis occur each year in the US, making it one of the most prevalent sexually transmitted diseases. (1) This disease may be underreported, largely as a result of substantial numbers of asymptomatic persons whose infections are not identified because screening is not available/ In addition, many females with mucopurulent cervicitis are asymptomatic. In some series, C trachomatis has been identified as the causative agent in up to 50% of women with pelvic inflammatory disease.
Reiter's syndrome is a multisystem disease commonly triggered by a genitourinary or bacterial enteric infection. (2) The incidence of Reiter's syndrome is estimated to be 3,5 per 100,000 in the US population. (3) Up to 85% of patients with Reiter's syndrome possess the HLA-B27 antigen. (4) However, the true incidence of Reiter's syndrome is debated because of the protean nature of its symptoms, as well as a lack of consensus in defining the syndrome.
The numbers of cases of Reiter's syndrome caused from C trachomatis genitourinary infections are equally difficult to document. In some reports, silent cystitis and cervicitis without urethritis may be the only evidence of urogenital involvement. (5)
The authors have no conflicts of interest to report. Corresponding author: Joseph M. Mazziotta, MD, Associate Director Tallahassee Memorial Family Practice Residency Program, 1301 Hodges Drive, Tallahassee, FL 32308. E-mail: mazziott-j@mail.tmh.org.
Joseph M. Mazziotta, MD, and Nighat Ahmed, MD Tallahassee Memorial Family Practice Residency Program, Tallahassee, Fla
Richard P. Usatine, Feature Editor Department of Family and Community Medicine, University of Texas Health Science Center at San Antonio
COPYRIGHT 2004 Dowden Health Media, Inc.
COPYRIGHT 2004 Gale Group