Definition
Tay-Sachs disease is a genetic disorder. A missing enzyme results in the accumulation of a fatty substance in the nervous system. This results in disability and death.
Description
Gangliosides are a fatty substance necessary for the proper development of the brain and nerve cells (nervous system). Under normal conditions, gangliosides are continuously broken down, so that an appropriate balance is maintained. In Tay-Sachs disease, the enzyme necessary for removing excess gangliosides is missing. This allows gangliosides to accumulate throughout the brain, and is responsible for the disability associated with the disease.
Tay-Sachs disease is particularly common among Jewish people of eastern European and Russian (Ashkenazi) origin. About one out of every 3,600 babies born to Ashkenazi Jewish couples will have the disease. Tay-Sachs is also more common among certain French-Canadian and Cajun French families.
Causes & symptoms
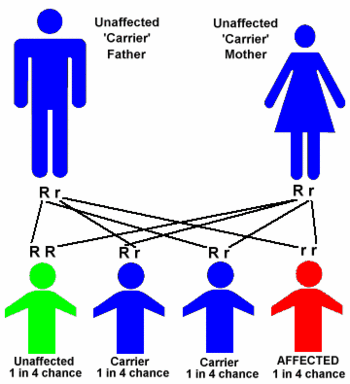
Tay-Sachs is a genetic disease, caused by a defective gene. Genes are located on chromosomes, and serve to direct specific development/processes within the body. Because it is a recessive disorder, only people who receive two defective genes (one from the mother and one from the father) will actually have the disease. People who have only one defective gene and one normal gene are called carriers. They carry the defective gene and thus the possibility of passing the gene and/or the disease on to their offspring.
The genetic defect in Tay-Sachs disease results in the lack of an important enzyme, called hexosaminidase A. Without this enzyme, gangliosides cannot be degraded. They build up within the brain, interfering with nerve functioning.
Classic Tay-Sachs disease strikes infants around the age of six months. Up until this age, the baby will appear to be developing normally. When Tay-Sachs begins to show itself, the baby will stop interacting with other people, and develop a staring gaze. Normal levels of noise will startle the baby to an abnormal degree. By about a year of age, the baby will have very weak, floppy muscles, and may be completely blind. The head will be quite large. Seizures become a problem between ages one and two , and the baby usually dies by about age four.
A few variations from this classical progression of Tay-Sachs disease are possible:
- Juvenile hexosaminidase A deficiency. Symptoms appear between ages two and five; the disease progresses more slowly, with death by about 15 years.
- Chronic hexosaminidase A deficiency. Symptoms may begin around age five, or may not occur until age 20-30. The disease is milder. Speech becomes slurred. The individual may have difficulty walking due to weakness, muscle cramps, and decreased coordination of movements. Some individuals develop mental illness. Many have changes in intellect, hearing, or vision.
Diagnosis
Examination of the eyes of a child with Tay-Sachs disease will reveal a very characteristic cherry-red spot at the back of the eye. Tests to determine the presence and quantity of hexosaminidase A can be performed on the blood, specially treated skin cells, or white blood cells. A carrier will have about half of the normal level of hexosaminidase A present, while a victim of the disease will have none.
Treatment
There is no treatment for Tay-Sachs disease.
Prognosis
Sadly, the prognosis for a child with classic Tay-Sachs disease is certain death. Because the so-called chronic form of Tay-Sachs has been discovered recently, prognosis for this type of the disease is not completely known.
Prevention
Prevention involves identifying carriers of the disease, and giving them sound information about the chance of their offspring having Tay-Sachs disease. When the levels of hexosaminidase A are half of normal, a person is a carrier of the defective gene. When a carrier and a non-carrier have children, none of their children will actually have Tay-Sachs. It is likely that 50% of their children will be carriers themselves. When two carriers have children, their children have a 25% chance of having normal genes, a 50% chance of being carriers of the defective gene, and a 25% chance of having two defective genes. The two defective genes cause the disease itself.
When a woman is already pregnant, tests can be performed on the either the cells of the baby or the placenta to determine whether the baby will have Tay-Sachs disease.
Key Terms
- Ganglioside
- A fatty (lipid) substance found within the brain and nerve cells.
Further Reading
For Your Information
Books
- Nelson Textbook of Pediatrics, edited by Richard Behrman. Philadelphia: W.B. Saunders Co., 1996.
Periodicals
- Motulsky, Arno G. "Screening for Genetic Disease." The New England Journal of Medicine, 336 (18)(May 1, 1997): 1314+.
- Rosebush, Patricia I. "Late-Onset Tay-Sachs Disease Presenting as Catatonic Schizophrenia: Diagnostic and Treatment Issues." The Journal of the American Medical Association, 274 (22)(December 13, 1995): 1744.
Organizations
- Late Onset Tay-Sachs Foundation. 1303 Paper Mill Road, Erdenheim, PA 19038. (800)672-2022.
- March of Dimes Birth Defects Foundation. National Office. 1275 Mamaroneck Avenue, White Plains, NY 10605. http://222.modimes.org.
- National Tay-Sachs and Allied Diseases Association, Inc. 2001 Beacon Street, Suite 204, Brookline, MA 02146. (800)672-2022.
Gale Encyclopedia of Medicine. Gale Research, 1999.