In this article, the evidence supporting different treatments for acute bacterial rhinosinusitis (ABRS) is reviewed. In part one (1) of this two-part article, clinical criteria for evaluating ABRS are described.
Antibiotics
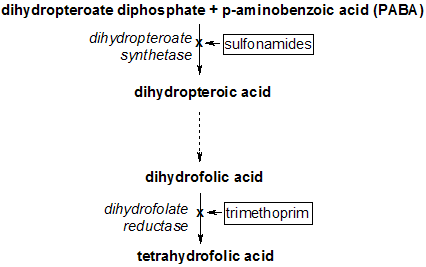
About two thirds of patients with ABRS improve without antibiotic treatment, and most patients with viral upper respiratory infection (URI) improve within seven days. (2) Antibiotic therapy should be reserved for patients who have had symptoms for more than seven days and who present with two or more clinical criteria for ABRS (purulent nasal discharge, maxillary tooth or facial pain [especially unilateral], unilateral maxillary sinus tenderness, or worsening symptoms after initial improvement), or for those with severe symptoms (3) (Figure 1).
[FIGURE 1 OMITTED]
RESULTS OF CLINICAL TRIALS
There have been no randomized controlled trials (RCTs) of antibiotic treatment for ABRS using sinus aspirate cultures before and after treatment, although nonrandomized trials have demonstrated bacteriologic cures. Five RCTs and two meta-analyses have compared antibiotics, usually amoxicillin and trimethoprim-sulfamethoxazole (TMP-SMX; Bactrim, Septra), with placebo, with clinical improvement as the outcome, which is the more clinically relevant patient-oriented outcome. (4,5) About 47 percent of patients treated with antibiotics and 32 percent of the control group were cured at 10 to 14 days. Eighty-one percent of patients treated with antibiotics and 66 percent of the control group were cured or improved, meaning one patient benefited for every seven treated with antibiotics. The treatment effect in these trials may have been underestimated because the lack of specificity of diagnosis diluted the effect of treatment.
Amoxicillin-clavulanate potassium (Augmentin), cephalosporins (cefuroxime [Ceftin] and cefixime [Suprax]), and macrolides (azithromycin [Zithromax] and clarithromycin [Biaxin]), have been studied extensively. (6,7) All have demonstrated similar clinical success rates--generally above 85 percent. The use of fluoroquinolones for ABRS is relatively new. Ciprofloxacin (Cipro) and cefuroxime had 90 percent resolution rates when administered to patients in a primary care setting. (8) In an open-label RCT, levofloxacin (Levaquin) and clarithromycin had 96 and 93 percent clinical success rates, respectively. (9)
Four meta-analyses published within the past seven years concluded that newer broad-spectrum antibiotics are no more effective than narrow-spectrum antibiotics. (4,5,10,11) In most of these studies, amoxicillin was compared with a cephalosporin, a fluoroquinolone, or a macrolide. The rapid emergence of antibiotic-resistant organisms associated with ABRS has made choosing an antibiotic more difficult. Surveillance studies have shown an increasing prevalence of antibiotic-resistant Streptococcus pneumoniae. (12,13) Up to 25 percent of these bacteria are penicillin resistant, and 15 percent are penicillin intermediate. Resistance to macrolides, doxycycline (Vibramycin), and TMP-SMX is common. (12) The prevalence of beta-lactamase-producing Haemophilus influenzae is about 30 percent, and resistance to TMP-SMX is common. (12) Nearly all Mycobacterium catarrhalis isolates produce beta-lactamase.
SELECTING AN ANTIBIOTIC
To integrate current antibiotic resistance surveillance data into antibiotic recommendations, the Sinus and Allergy Health Partnership (SAHP) used the Poole Therapeutic Outcomes Model, a mathematical model that predicts clinical efficacy for each of the antibiotics commonly prescribed for ABRS (Table 1). (13-16) The model incorporates assumptions about the probability of bacterial infection, pathogen distribution, spontaneous resolution rates, and in vitro activity of antibiotics. (15)
When choosing antibiotic therapy for ABRS, physicians should consider recent antibiotic use, efficacy, and cost. The SAHP guidelines classify patients with ABRS into two groups to determine initial treatment: (1) those with mild symptoms who have not received antibiotics within six weeks and (2) those who have moderately severe disease or have received antibiotics within six weeks. (16) Patients with moderate disease are considered less likely to have spontaneous resolution and thus have a higher rate of treatment failure. The guidelines offer no criteria for severity. The categorization of moderate or mild severity is left to the physician's clinical judgment, but an example was offered with earlier recommendations that emphasized the inflammatory signs of fever and tenderness. (17)
Although lacking complete H. influenzae coverage, amoxicillin is still a good choice for a first-line antibiotic in community-acquired ABRS because many infections with resistant organisms improve anyway,18 and because it is well tolerated and inexpensive (Table 1). (13-16) Higher daily doses of amoxicillin (3 to 4 g per day) may be necessary in areas with a high prevalence of penicillin-resistant S. pneumoniae. TMP-SMX and doxycycline are alternatives for use in patients who are allergic to beta lactams, but they have limited coverage for H. influenzae and S. pneumoniae, and failure rates of up to 25 percent are possible.16 Erythromycin, second-generation cephalosporins with less activity against H. influenzae (e.g., cefaclor [Ceclor], cefprozil [Cefzil], loracarbef [Lorabid]), and tetracycline should not be used to treat ABRS. (19)
Although the cephalosporins (cefpodoxime [Vantin], cefuroxime, cefdinir [Omnicef], ceftriaxone [Rocephin]) and amoxicillin/clavulanate potassium also have been recommended for initial treatment, (16) any benefit of these agents as initial therapy must be balanced against their much higher cost and concerns about increasing antibiotic resistance in the community. A retrospective cohort study of a pharmaceutical database of 29,000 adults with ABRS showed equivalent success rates with the use of older, inexpensive antibiotics at one half the cost. (20) A cost-effectiveness analysis showed that even if more expensive agents were 23 percent more effective than amoxicillin, using them empirically would be cost effective only if the prevalence of true bacterial sinusitis in treated patients was greater than 80 percent. (21)
Second-line antibiotics should be considered when the patient has moderate disease, has used antibiotics in the past six weeks, or has no response to treatment within 72 hours. Amoxicillin-clavulanate potassium and f luoroquinolones (gatif loxacin [Tequin], levofloxacin, and moxifloxacin [Avelox]) currently have the best coverage for H. influenzae and S. pneumoniae. Other choices include intramuscular ceftriaxone or combination therapies including high-dose amoxicillin; clindamycin (Cleocin) plus cefixime; or high-dose amoxicillin or clindamycin plus rifampin (Rifadin). (16) In patients with a history of beta-lactam allergies, the use of fluoroquinolones or combination therapy with clindamycin and rifampin has been recommended. (16)
DURATION OF TREATMENT
Most clinical trials have used 10- to 14-day courses of antibiotic therapy. Sinus puncture studies have shown eradicated pathogens in at least 95 percent of patients after a 10-day course of antibiotics. (22) Results of one study showed no differences in clinical or radiographic improvement between patients receiving three- or 10-day courses of TMPSMX. 23 However, this study was conducted before 1995, and microbial resistance patterns have changed since then. More recently, five-day treatment courses with azithromycin and telithromycin (Ketek) were found to be effective. (24,25)
TREATMENT FAILURE
When a patient fails to respond to therapy, additional history, physical examination, cultures, or imaging may be necessary. If a change in antibiotic therapy is made, the limitations in coverage of the initial antibiotic should be considered. A switch to a fluoroquinolone is recommended after failure of amoxicillin or doxycycline. (16) Combination therapy may be advantageous, particularly in patients previously treated with cefdinir or macrolides.
Ancillary Treatment
The evidence supporting the use of ancillary treatment for ABRS is relatively weak (Table 2). (26-48) Some studies show improvement in symptoms, but no treatments have been shown to affect the duration of illness. (26-28) Oral decongestants can be used until symptoms resolve. In patients with stable hypertension, decongestants have not been shown to seriously increase blood pressure. (29) Decongestants should be used with caution in patients with ischemic heart disease, glaucoma, or prostatic hypertrophy.
Although topical decongestants have been advocated in the past, their use is more controversial. Symptoms are improved in some patients, but reduced mucosal blood flow may increase inflammation. (30) Topical decongestants should not be used longer than three days to avoid rebound vasodilation.
No clinical studies support the use of antihistamines for treatment of patients with ABRS. Even though histamine does not play a role in this infectious condition except, possibly, in patients who also have a predisposing allergic rhinitis, these drugs have some anti-inflammatory effects that may be beneficial.31 However, the anticholinergic effects of first-generation antihistamines could impair clearance by thickening mucus. (31) Newer second-generation antihistamines have little or no anticholinergic effect and may have a role in treatment of patients with allergy and chronic sinusitis, but are not recommended for ABRS. (48)
The topical anticholinergic agent ipratropium bromide (Atrovent) has been used to decrease rhinorrhea in patients with the common cold, (32) but there are no studies in patients with ABRS. Theoretically, ipratropium may increase the viscosity of mucus and impair its clearance, but this effect appears to be less prominent with ipratropium than with antihistamines. (31)
Most studies of intranasal steroids in patients with ABRS have not shown an effect on clinical outcomes. These studies often were underpowered and included patients who had chronic sinusitis and nasal polyposis, as well as ABRS. (33-36) A recent RCT, (37) limited to patients with a history of previous recurrent or chronic sinusitis, compared fluticasone (Flovent) with placebo in the treatment of patients with ABRS. Both groups received cefuroxime and topical xylometazoline (Otrivin) for three days. Patients who received fluticasone showed more rapid improvement (6.0 versus 9.5 days) than patients who received placebo.
Nasal saline spray, nasal irrigation, and mist humidification have been recommended in the past to promote mucociliary clearance by decreasing congestion, moistening the nasal cavity, and removing crusty mucus. (31) Most trials have been small, many were not controlled, and methods varied, so evidence supporting their use is only fair. (27,28,38) Saline irrigation is safe, and there are no documented serious adverse effects. (38) Hypertonic saline irrigation improved symptoms and decreased medication use in patients with chronic sinusitis. (39,40) Saline sprays have been shown to reduce symptoms of rhinitis, (41) but there are no studies in patients with ABRS. Controlled studies of mist use in URI have not shown a benefit. (42,43)
Guaifenesin (Hytuss), a mucolytic agent, should improve mucus clearance by thinning secretions, but there is no evidence of clinical benefit. An RCT showed no effect on mucociliary clearance in healthy subjects. (44) However, guaifenesin did reduce nasal congestion in an RCT of patients infected with human immunodeficiency virus who had acute or chronic rhinosinusitis. (45)
There is insufficient evidence to recommend the use of vitamin C, zinc salt lozenges, or echinacea in patients with ABRS. Using the outcome of cold symptoms after seven days, a meta-analysis of eight clinical trials of zinc salt-lozenge treatment for the common cold did not find a significant benefit (odds ratio, 0.50; 95 percent confidence interval, 0.19 to 1.29).46 Several trials of echinacea extract in the treatment of the common cold reported a mild benefit, but each trial had serious methodologic flaws. A recent RCT of echinacea in college students with common colds showed no benefit. (47)
Complications and Referral
Patients with complications or treatment failure after extended antibiotic therapy should be referred to an otolaryngologist (Table 3). (6,48) Patients who are referred to otolaryngologists usually are evaluated with nasal endoscopy and a sinus computed tomographic scan. Patients with frequent recurrences of ABRS and inadequately controlled allergic rhinitis should be referred to an allergist for consideration of immunotherapy.
TABLE 3
Indications for Referral in Patients with Bacterial Rhinosinusitis
Findings of severe acute bacterial rhinosinusitis Complications Periorbital cellulitis Intracranial abscess Meningitis Cavernous sinus thrombosis Pott's puffy tumor (infectious erosion of the ethmoid or frontal sinus)
Anatomic defects causing obstruction Treatment failure after extended course of antibiotics
Frequent recurrences (more than three episodes per year)
Nosocomial infections
Immunocompromised host
Biopsy to rule out granulomatous disease, neoplasms, or fungal infections
Evaluation for immunotherapy of allergic rhinitis Information from references 6 and 48.
REFERENCES
(1.) Scheid DC, Hamm RM. Acute bacterial rhinosinusitis in adults: part I. Evaluation. Am Fam Physician 2004;70:1685-92.
(2.) Axelsson A, Chidekel N, Grebelius N, Jensen C. Treatment of acute maxillary sinusitis. A comparison of four different methods. Acta Otolaryngol 1970;70:71-6.
(3.) Hickner JM, Bartlett JG, Besser RE, Gonzales R, Hoffman JR, Sande MA. Principles of appropriate antibiotic use for acute rhinosinusitis in adults: background. Ann Intern Med 2001;134:498-505.
(4.) Williams JW Jr, Aguilar C, Cornell J, Chiquette ED, Dolor RJ, Makela M, et al. Antibiotics for acute maxillary sinusitis. Cochrane Database Syst Rev 2004;(2): CD000243.
(5.) Diagnosis and treatment of acute bacterial rhinosinusitis. Evid Rep Technol Assess (Summ) 1999;9:1-5.
(6.) Poole MD. A focus on acute sinusitis in adults: changes in disease management. Am J Med 1999;106:38S-47S.
(7.) Low DE, Desrosiers M, McSherry J, Garber G, Williams JW Jr, Remy H, et al. A practical guide for the diagnosis and treatment of acute sinusitis. CMAJ 1997;156(suppl6):S1-14.
(8.) Weis M, Hendrick K, Tillotson G, Gravelle K. Multicenter comparative trial of ciprofloxacin versus cefuroxime axetil in the treatment of acute rhinosinusitis in a primary care setting. Rhinosinusitis Investigation Group. Clin Ther 1998;20:921-32.
(9.) Kahn JB, Rielly-Bauvin K, Demartin EL, et al. Multicenter, open-label, randomized study to compare the safety and efficacy of oral levofloxacin and Biaxin in the treatment of acute maxillary sinusitis in adults. Abstracts from the Proceedings of the 35th Annual Meeting of the IDSA, San Francisco, September 13-18, 1997. Abstract 578.
(10.) De Bock GH, Dekker FW, Stolk J, Springer MP, Kievit J, van Houwelingen JC. Antimicrobial treatment in acute maxillary sinusitis: a meta-analysis. J Clin Epidemiol 1997;50:881-90.
(11.) De Ferranti SD, Ioannidis JP, Lau J, Anninger WV, Barza M. Are amoxycillin and folate inhibitors as effective as other antibiotics for acute sinusitis? A meta-analysis. BMJ 1998;317:632-7.
(12.) Jacobs MR, Felmingham D, Appelbaum PC, Gruneberg RN. The Alexander Project 1998-2000: susceptibility of pathogens isolated from community-acquired respiratory tract infection to commonly used antimicrobial agents. J Antimicrob Chemother 2003;52:229-46.
(13.) Karlowsky JA, Draghi DC, Thornsberry C, Jones ME, Critchley IA, Sahm DF. Antimicrobial susceptibilities of Streptococcus pneumoniae, Haemophilus influenzae and Moraxella catarrhalis isolated in two successive respiratory seasons in the US. Int J Antimicrob Agents 2002;20:76-85.
(14.) Marchant CD, Carlin SA, Johnson CE, Shurin PA. Measuring the comparative efficacy of antibacterial agents for acute otitis media: the "Pollyanna phenomenon." J Pediatr 1992;120:72-7.
(15.) Poole MD. A mathematical therapeutic outcomes model for sinusitis. Otolaryngol Head Neck Surg 2004;130(1 suppl):46-50.
(16.) Anon JB, Jacobs MR, Poole MD, Ambrose PG, Benninger MS, Hadley JA, et al. Antimicrobial treatment guidelines for acute bacterial rhinosinusitis. Otolaryngol Head Neck Surg 2004;130(1 suppl):1-45.
(17.) Antimicrobial treatment guidelines for acute bacterial rhinosinusitis. Sinus and Allergy Health Partnership. Otolaryngol Head Neck Surg 2000;123(1 pt 2):5-31.
(18.) Gwaltney JM Jr, Sydnor A Jr, Sande MA. Etiology and antimicrobial treatment of acute sinusitis. Ann Otol Rhinol Laryngol Suppl 1981;90(3 pt 3):68-71.
(19.) Gwaltney JM Jr, Jones JG, Kennedy DW. Medical management of sinusitis: educational goals and management guidelines. The International Conference on Sinus Disease. Ann Otol Rhinol Laryngol Suppl 1995;167:22-30.
(20.) Piccirillo JF, Mager DE, Frisse ME, Brophy RH, Goggin A. Impact of first-line vs second-line antibiotics for the treatment of acute uncomplicated sinusitis. JAMA 2001;286:1849-56.
(21.) Balk EM, Zucker DR, Engels EA, Wong JB, Williams JW Jr, Lau J. Strategies for diagnosing and treating suspected acute bacterial sinusitis: a cost-effectiveness analysis. J Gen Intern Med 2001;16:701-11.
(22.) Gwaltney JM Jr, Scheld WM, Sande MA, Sydnor A. The microbial etiology and antimicrobial therapy of adults with acute community-acquired sinusitis: a fifteen-year experience at the University of Virginia and review of other selected studies. J Allergy Clin Immunol 1992;90(3 pt 2):457-61.
(23.) Williams JW Jr, Holleman DR Jr, Samsa GP, Simel DL. Randomized controlled trial of 3 vs 10 days of trimethoprim/ sulfamethoxazole for acute maxillary sinusitis. JAMA 1995;273:1015-21.
(24.) Klapan I, Culig J, Oreskovic K, Matrapazovski M, Radosevic S. Azithromycin versus amoxicillin/clavulanate in the treatment of acute sinusitis. Am J Otolaryngol 1999;20:7-11.
(25.) Roos K, Brunswig-Pitschner C, Kostrica R, Pietola M, Leroy B, Rangaraju M, et al. Efficacy and tolerability of once-daily therapy with telithromycin for 5 or 10 days for the treatment of acute maxillary sinusitis. Chemotherapy 2002;48:100-8.
(26.) Smith MB, Feldman W. Over-the-counter cold medications. A critical review of clinical trials between 1950 and 1991. JAMA 1993;269:2258-63.
(27.) Zeiger RS. Prospects for ancillary treatment of sinusitis in the 1990s. J Allergy Clin Immunol 1992;90(3 pt 2):478-95.
(28.) Mabry RL. Therapeutic agents in the medical management of sinusitis. Otolaryngol Clin North Am 1993;26:561-70.
(29.) Bravo EL. Phenylpropanolamine and other over-the-counter vasoactive compounds. Hypertension 1988;11(3 pt 2):117-10.
(30.) Bende M, Fukami M, Arfors KE, Mark J, Stierna P, Intaglietta M. Effect of oxymetazoline nose drops on acute sinusitis in the rabbit. Ann Otol Rhinol Laryngol 1996;105:222-5.
(31.) Benninger MS, Anon J, Mabry RL. The medical management of rhinosinusitis. Otolaryngol Head Neck Surg 1997;117(3 pt 2):S41-9.
(32.) Hayden FG, Diamond L, Wood PB, Korts DC, Wecker MT. Effectiveness and safety of intranasal ipratropium bromide in common colds. A randomized, double-blind, placebo-controlled trial. Ann Intern Med 1996;125:89-97.
(33.) Krouse HA, Phung ND, Klaustermeyer WB. Intranasal beclomethasone in severe rhinosinusitis and nasal polyps. Ann Allergy 1983;50:385-8.
(34.) Cuenant G, Stipon JP, Plante-Longchamp G, Baudoin C, Guerrier Y. Efficacy of endonasal neomycin-tixocortol pivalate irrigation in the treatment of chronic allergic and bacterial sinusitis. ORL J Otorhinolaryngol Relat Spec 1986;48:226-32.
(35.) Qvarnberg Y, Kantola O, Salo J, Toivanen M, Valtonen H, Vuori E. Influence of topical steroid treatment on maxillary sinusitis. Rhinology 1992;30:103-12.
(36.) Meltzer EO, Orgel HA, Backhaus JW, Busse WW, Druce HM, Metzger WJ, et al. Intranasal flunisolide spray as an adjunct to oral antibiotic therapy for sinusitis. J Allergy Clin Immunol 1993;92:812-23.
(37.) Dolor RJ, Witsell DL, Hellkamp AS, Williams JW Jr, Califf RM, Simel DL. Comparison of cefuroxime with or without intranasal fluticasone for the treatment of rhinosinusitis. The CAFFS Trial: a randomized controlled trial. JAMA 2001;286:3097-105.
(38.) Papsin B, McTavish A. Saline nasal irrigation: its role as an adjunct treatment. Can Fam Physician 2003;49:168-73.
(39.) Rabago D, Zgierska A, Mundt M, Barrett B, Bobula J, Maberry R. Efficacy of daily hypertonic saline nasal irrigation among patients with sinusitis: a randomized controlled trial. J Fam Pract 2002;51:1049-55.
(40.) Heatley DG, McConnell KE, Kille TL, Leverson GE. Nasal irrigation for the alleviation of sinonasal symptoms. Otolaryngol Head Neck Surg 2001;125:44-8.
(41.) Nuutinen J, Holopainen E, Haahtela T, Ruoppi P, Silvasti M. Balanced physiological saline in the treatment of chronic rhinitis. Rhinology 1986;24:265-9.
(42.) Hendley JO, Abbott RD, Beasley PP, Gwaltney JM Jr. Effect of inhalation of hot humidified air on experimental rhinovirus infection. JAMA 1994;271:1112-3.
(43.) Forstall GJ, Macknin ML, Yen-Lieberman BR, Medendrop SV. Effect of inhaling heated vapor on symptoms of the common cold. JAMA 1994;271:1109-11.
(44.) Sisson JH, Yonkers AJ, Waldman RH. Effects of guaifenesin on nasal mucociliary clearance and ciliary beat frequency in healthy volunteers. Chest 1995;107:747-51.
(45.) Wawrose SF, Tami TA, Amoils CP. The role of guaifenesin in the treatment of sinonasal disease in patients infected with the human immunodeficiency virus (HIV). Laryngoscope 1992;102:1225-8.
(46.) Jackson JL, Peterson C, Lesho E. A meta-analysis of zinc salts lozenges and the common cold. Arch Intern Med 1997;157:2373-6.
(47.) Barrett BP, Brown RL, Locken K, Maberry R, Bobula JA, D'Alessio D. Treatment of the common cold with unrefined echinacea. A randomized, double-blind, placebo-controlled trial. Ann Intern Med 2002;137:939-46.
(48.) Spector SL, Bernstein IL, Li JT, Berger WE, Kaliner MA, Schuller DE, et al. Parameters for the diagnosis and management of sinusitis. J Allergy Clin Immunol 1998;102(6 pt 2):S107-44.
Antibiotic therapy should be reserved for use in patients who have had symptoms for more than seven days and who meet two or more clinical criteria for acute bacterial rhinosinusitis.
This is part II of a two-part article on bacterial sinusitis in adults. Part I, "Evaluation," appears in this issue of AFP on page 1685.
* Patient information: A handout on sinus infections, written by the authors of this article, is provided on page 1711. See page 1621 for definitions of strength-of-recommendation labels.
Members of various medical faculties develop articles for "Practical Therapeutics." This article is one in a series coordinated by the Department of Family and Preventive Medicine at University of Oklahoma Health Sciences Center, Tulsa, Okla. Coordinator of the series is John Tipton, M.D.
The authors indicate that they do not have any conflicts of interest. Sources of funding: none reported.
DEWEY C. SCHEID, M.D., M.P.H., and ROBERT. M. HAMM, PH.D. University of Oklahoma Health Sciences Center, Oklahoma City, Oklahoma
COPYRIGHT 2004 American Academy of Family Physicians
COPYRIGHT 2004 Gale Group