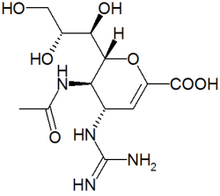
Zanamivir may help to fight potential flu epidemic
EDITOR--The zanamivir issue described by Yamey in his news article[1] and the whole subject of treating influenza have ramifications apart from the potential expense to the British taxpayer (who can easily turn into a patient).
I am keen on any development that might help to reduce the burden of disease in hospital wards. If I were asked to state which single condition will fill up my inpatient beds and send healthcare staff home ill most efficiently, I would always choose influenza. Although it is true that influenza is often a mild illness, its association with the development of potentially lethal sequelae is well recognised. It has been described as the best known model of bacterial-viral coinfection.[2] Influenza is a powerful predisposing factor for invasive meningococcal disease[3] one of the few bacterial conditions still regularly killing otherwise normal healthy young people in the United Kingdom. Hubert et al have stated that when an epidemic of influenza-like syndrome is identified, medical practitioners should be informed of the likelihood of mi increased incidence and severity of meningococcal disease.[4] We cannot currently vaccinate against Neisseria meningitidis type B. Zanamivir has the potential to be useful here. This certainly needs further investigation.
Influenza epidemics result in increased hospital admission rates for bacterial pneumonia,[2] and I have come across many patients who have known the pain and misery of having to have chest drains inserted for the drainage of empyemas as a consequence of having suffered a bout of "not very serious" influenza.
The zanamivir issue merits a broader debate, which should not centre exclusively upon whether or not it will be a helpful agent for groups at high risk. At a recent meeting in Geneva, to mark the 50th anniversary of WHO influenza surveillance, the Director General, Gro Harlem Brundtland, said that, "time to react may be very short--from the first recognition of a new subtype and the onset of a full-blown pandemic, it may be too short to prepare a vaccine and to use it."[5]
We have time to plan now but may not later. Like the little Dutch boy, we may need a finger to stick in the dyke to stop everyone drowning--perhaps zanamivir and similar drugs are that finger.
Stephen T Green consultant physician in infectious diseases and tropical medicine
Royal Hallamshire Hospital, Sheffield S10 2JF Steve.Green@csuh.nhs.uk
Competing interest: STG has received fees for lecturing from GlaxoWellcome.
[1] Yamey G. NICE to rule on influenza drug zanamivir. BMJ 1999:319;937. (9 October.)
[2] Floret D. Virus-bacteria co-infections. Arch Pediatr 1997;4:1119-24.
[3] Stuart JM, Cartwright K, Andrews NJ. Respiratory syncytial virus infection and meningococcal disease. Epidemiol Infect 1996;117:107-11.
[4] Hubert B, Watier L, Garnerin P, Richardson S. Meningococcal disease and influenza-like syndrome: a new approach to an old question. J Infect Dis 1992;166:542-5.
[5] World Health Organisation. 50 years of influenza surveillance: much still to do to stop a common killer. Geneva: WHO, 1990. (Press release WHO/11.)
NHS regulations are of questionable legality
EDITOR--As Yamey points out in his news article, the National Institute for Clinical Excellence considers that zanamivir (Relenza) is not cost effective and so will very closely monitor its use by doctors in NHS practice.[1] In reality this is a total ban, enforced by threat rather than by legislation. Since general practitioners are not permitted to provide any drug or treatment privately to their NHS patients I wonder what sort of service our patients will receive when this philosophy is taken to its logical conclusion and doctors are required to pay for all the treatments their patients need under the NHS conditions and terms of their service. This is the logical end point of the many recent primary care initiatives.
It may be appropriate to restrict NHS funding for sildenafil (Viagra) as a lifestyle drug, but zanamivir seems to be a potentially lifesaving treatment that might benefit most of the UK's population, particularly when the next influenza epidemic arrives.
All members of our society supposedly have access to free NHS medical care, but this provision is now overtly rationed, and a large number of treatments are simply not available owing to lack of funds. The moderately wealthy, including politicians, can afford medical insurance with instant access to specialist care in sumptuous surroundings. NHS rationing, however, applies to the productive majority of Middle England who are in work but who do not have, or cannot afford, medical insurance or a consultant's private fees. These are the very patients who might wish to pay their doctor a reasonable fee for the many procedures or drugs that the state is no longer prepared to provide for them. They already subsidise the NHS, paying 5.90 [pounds sterling] per item in prescription charges, and they may wish to purchase zanamivir directly from me if it only meant fewer very costly days off work owing to sickness. This is an option apparently denied to them.[2]
I have not abandoned the medical ethic. I believe a doctor's duty is to treat each of his or her patients to the best of his or her ability, and so he or she can take no part in rationing decisions, including the management of the local NHS primary care group. I also consider the prohibition of effective medical treatments to be morally as unacceptable as the Poor Laws of the nineteenth century. It echoes the ethics of an internment camp.
It may even be illegal.
P D Thomas general practitioner and dispensing doctor Gipping Valley Practice, Barham, Suffolk IP6 0AS Competing interest: None declared.
[1] Yamey G. NICE to rule on influenza drug zanamivir. BMJ 1999:319;937. (9 October.)
[2] Thomas PD. NHS Regulations deny patients cheap drugs. BMJ 1993;306:1748-9.
Advice to authors
We prefer to receive all responses electronically, sent either directly to our website or to the editorial office as email or on a disk. Processing your letter will be delayed unless it arrives in an electronic form.
We are now posting all direct submissions to our website within 24 hours of receipt and our intention is to post all other electronic submissions there as well. All responses will be eligible for publication in the paper journal.
Responses should be under 400 words and relate to articles published in the preceding month. They should include [is less than or equal to] 5 references, in the Vancouver style, including one to the BMJ article to which they relate. We welcome illustrations.
Please supply each author's current appointment and full address, and a phone or fax number or email address for the corresponding author. We ask authors to declare any competing interest. Please send a stamped addressed envelope if you would like to know whether your letter has been accepted or rejected.
Letters will be edited and may be shortened.
www.bmj.com letters@bmj.com
COPYRIGHT 2000 British Medical Association
COPYRIGHT 2000 Gale Group