Diabetes mellitus is a chronic condition whereby there is insufficient insulin to meet the body's needs. This results in a decreased ability to clear blood sugar (glucose) efficiently from the bloodstream. The problem can be due to decreased secretion of insulin; a problem with the release of insulin; insulin that cannot properly stimulate insulin receptors on the cells that require it (insulin resistance); or insulin that is inactivated before it is able to function.
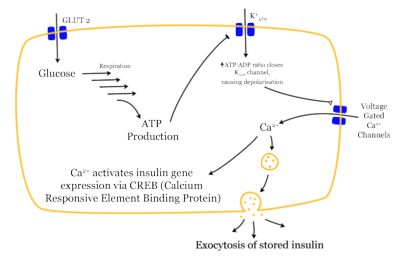
Insulin is a hormone produced by the beta cells in the pancreas. Once released into the bloodstream, insulin allows glucose (blood sugar) to be transported into the cells, to be used primarily for energy production. After consumption of a meal containing carbohydrates, blood sugar increases. In response to rising blood sugar levels, insulin is released by the pancreas, which enables the cells of the body to extract glucose (sugar) from the bloodstream. As such, insulin decreases blood sugar and provides cells with the glucose they require for energy production.
Insulin resistance appears to represent the first stage of diabetes and a prediabetic state. Blood sugar remains elevated, even though the pancreas is still producing insulin. In response to this elevated blood sugar, the pancreas releases even more insulin, and hyperinsulinemia (too much insulin in the blood) occurs. Eventually, the cells that make insulin in the pancreas can "burn out" and insulin resistance may turn into the type of diabetes that requires insulin injections (type 1 diabetes).
The risk of developing type 2 diabetes appears to be associated with genetic defects. However, new evidence points to diet and lifestyle as important factors that may be responsible for the development of the disease. Research has shown a strong connection between upper-body obesity (people with "apple shapes") and the development of type 2 diabetes mellitus.
Most people with type 2 diabetes or prediabetes are overweight. Excess abdominal weight does not stop insulin formation, but it does make the body less sensitive to insulin. It has been shown that weight loss can reverse this problem.
Diabetes increases the risk of chronic conditions like heart disease; retinopathy (a disease of the retina) and blindness; peripheral neuropathies (a disease of the nervous system); circulation problems that can lead to amputation; problems with the immune system; and skin ulcers and poor wound healing.
Heart disease is the leading cause of diabetes-related deaths: The risk of death from heart disease is two to four times higher in diabetics compared to nondiabetics. The risk of stroke is two to four times higher in people with diabetes. Patients with diabetes develop more atherosclerosis (hardening of the arteries) than people without diabetes, and 60 percent to 65 percent of patients with diabetes have high blood pressure.
Dietary and Lifestyle Considerations
1. Lose weight and consume high-fiber foods: In most studies, type 2 diabetes has improved with weight loss. Additionally, most doctors recommend that people with diabetes reduce intake of sugar from snacks and processed foods, and that they replace these foods with high-fiber, whole foods.
A high-fiber diet has been shown to work quite well in controlling diabetes. Studies have shown that when diabetic subjects ingested a diet containing 50 grams per day of dietary fiber, exclusively through the consumption of foods naturally high in fiber - such as leafy green vegetables, granola, and fruit - their blood sugar and blood insulin levels dropped significantly, and there was a marked decrease in LDL-cholesterol (the bad cholesterol) and triglyceride levels (blood fats).
Fiber is the indigestible part of plant food that acts as roughage for the body. There are two types of fiber: Water-soluble fiber is found in fruits, vegetables, and legumes in the form of guar, pectin, and gums. These products form a gel in the gastrointestinal tract that allows for a food to be held there longer, causing a slow rise in blood sugar. This type of fiber also helps to lower cholesterol. Insoluble fiber is made of cellulose, hemicellulose and lignins, and can be found in grains and bran. This food also takes longer to be broken down and used for energy, but its main value is in adding bulk and preventing constipation
High-fiber supplements, such as psyllium, guar gum (found in beans) pectin (from fruit), and oat bran, have improved glucose tolerance in some studies
2. Consume more low-glycemicindex carbohydrates: Authorities also recommend lowering the glycemic index of the diet to improve the control of diabetes. Eating carbohydrate-containing foods, whether high in sugar or high in starch (such as bread, potatoes, processed breakfast cereals, and rice), temporarily raises blood sugar and insulin levels. Beans, peas, fruit, and oats have low glycemic-index values, in that their carbohydrates are absorbed more slowly and tend not to cause a sudden rise in blood sugar.
Almost all legumes (beans and peas) have a moderate glycemic index. They also provide a source of water-soluble fiber, which is valuable for lowering cholesterol.
Some vegetables have a high glycémie index and should be used in moderation in cases of diabetes or to improve a prediabetic state. These include white potatoes (baked), carrots, beets, and turnips. However, if an individual is eliminating other sources of refined sugar in the diet and is decreasing the amount of complex carbohydrates (breads and pastas), he or she should be able to eat these vegetables with moderation.
Fruits are generally middle of the road in terms of glycemic index; but dried fruits, which are concentrated, have a higher index. To lower the glycemic index and total calorie consumption from fruit juices, limit intake or dilute with three-fourths water.
Most sweeteners, such as honey, molasses, sugar, and white grape juice concentrate, tend to have a high glycemic index. Rice syrup and granulated rice sweeteners may be used as alternatives.
Grains such as rice, wheat and corn tend to have a high glycemic index, but buckwheat, millet, barley, rye and bulgur are actually quite low. For successful weight loss and blood sugar control, this group of foods should be used in moderation.
Vegetarians have been reported to have a low risk of type 2 diabetes. When people with diabetic nerve damage switched to a vegan diet (no meat, dairy or eggs), improvements were reported after only several days. In one trial, pain completely disappeared in 17 of 21 people.
3. Exercise: Consistent exercise helps decrease body fat and improves insulin sensitivity. People who exercise are less likely to develop type 2 diabetes than those who do not. Exercise can decrease the risk for heart problems in diabetic patients. Regular exercise can improve heart and lung health, make insulin work better, and increase HDL cholesterol while decreasing LDL cholesterol. Exercise also helps to regulate blood sugar. At a minimum, diabetics should get 30 minutes of some form of exercise at least four days a week.
4. Avoid alcohol: Some studies have reported that alcohol worsens glucose tolerance in people with diabetes. People with diabetes who drink also have been reported to have a high risk for eye and nerve damage.
5. Avoid smoking: People with diabetes who smoke have a higher risk for kidney damage, heart disease, and other diabetes-linked problems. Smokers also are more likely to develop diabetes.
Supplement Considerations
1. High-potency multiple vitamin/mineral: A high-potency multiple vitamin/mineral is defined as a supplement that is antioxidant-enriched and contains a B-50 complex and at least 500 mg of elemental calcium, in addition to standard levels of all vitamins and minerals from vitamin A to zinc. The antioxidant levels should be in the following range: vitamin A: 2,000-3,000 IU; vitamin C: 750-1,000 mg; vitamin E: 200-400IU; selenium: 100-200 meg; beta-carotene: 10,000-15,000 IU; lycopene powder: 5-10 mg; lutein powder: 5-10 mg; bioflavonoids: 50-75 mg.
In a double-blind study, supplementation with a multiple vitamin and mineral preparation for one year reduced the risk of infection by more than 80 percent in middle-aged and elderly diabetics, compared with a placebo group. Other reasons for diabetic and prediabetic patients to take a high-potency multiple vitamin and mineral include:
A. Chromium - Chromium helps insulin clear glucose from the bloodstream, allowing cells to burn glucose for energy.
B. Magnesium - Magnesium is involved in the breakdown of glucose and the release of insulin. Low magnesium levels may make diabetes worse in some people. Low magnesium in the blood occurs in about 25 percent of diabetic patients.
C. Zinc - Zinc deficiency is found in patients with blood sugar problems. In clinical studies, diabetic animals and humans with zinc deficiencies improved when supplemented with zinc. Zinc has been shown to regulate insulin production by the pancreas, and glucose use by muscle and fat cells.
D. Vitamin E - Supplementation with vitamin E has improved glucose tolerance in people with type 2 diabetes in most double-blind trials. Vitamin E also has improved glucose tolerance in elderly people without diabetes. Three months or more of supplementation may be required for benefits to become apparent. The amount used is at least 900 IU of vitamin E per day. (Note: A high-potency multiple vitamin ay have only 400 IU; thus, an additional vitamin E supplement should be considered to boost the daily supplementation level to 900-1,000 IU.) Vitamin E also may help reduce the risk of heart disease in diabetic individuals.
E. Vitamin C - People with type 1 diabetes appear to have low vitamin C levels. Vitamin C also lowers sorbitol in people with diabetes. Sorbitol is a sugar that can accumulate and damage the eyes, nerves, and kidneys of people with diabetes. Vitamin C may improve glucose tolerance in type 2 diabetes patients, although not every study confirms this benefit. Vitamin C supplementation (500 mg twice daily for one year) has significantly reduced urinary protein loss (proteinuria) in people with diabetes. Urinary protein loss is associated with poor prognosis in diabetes cases.
F. B Vitamins - Many people with diabetes have low blood levels of vitamin B6. Levels are even lower in people with diabetes who also have nerve damage (neuropathy). Biotin is a B vitamin that is also needed to process glucose.
Blood levels of vitamin B1 (thiamine) have been found to be low in people with type 1 diabetes. In one study, administration of both vitamin B1 (25 mg per day) and vitamin B6 (50 mg per day) led to significant improvement of symptoms of diabetic neuropathy after four weeks. Another trial found that combining vitamin B1 and vitamin B6 plus vitamin B12 led to improvement in some aspects of diabetic neuropathy in a 12-week trial.
Vitamin B12 is needed for normal functioning of nerve cells. Vitamin B12, taken orally, has reduced nerve damage caused by diabetes in most people studied.
G. Vitamin D - Vitamin D is needed to maintain adequate blood levels of insulin. Vitamin D receptors have been found in the pancreas, where insulin is made, and preliminary evidence suggests supplementation can increase insulin levels in some people with type 2 diabetes.
H. Manganese - People with diabetes may have low blood levels of manganese. Animal research suggests manganese deficiency can contribute to glucose intolerance and may be reversed by supplementation.
2. Essential fatty acids (combination of borage seed, flaxseed and fish oil) - The essential fatty acids from these medicinal oils provide the body with the raw materials for the production of local hormones (prostaglandin hormones) known to reduce risk of heart disease, support nerve function, skin health, and suppress inflammation.
3. Alpha-lipoic acid (ALA) - Alphalipoic acid is a fat-and water-soluble antioxidant made by the body. Supplementation with alpha-lipoic acid has been shown to be beneficial for some problems facing diabetics. It enhances glucose uptake in type 2 diabetes, inhibits glycosylation (the abnormal attachment of sugar to protein), and has been used to improve diabetic nerve damage and reduce pain associated with nerve damage.
4. Glucomannan - Glucomannan is a water-soluble dietary fiber derived from konjac root. Glucomannan delays stomach emptying, leading to a more gradual absorption of dietary sugar. This effect absorption of dietary sugar. This effect can reduce the elevation of blood sugar levels, which is typical after consuming a meal. Overall diabetic control has been shown to improve with glucomannan-enriched diets, according to clinical trials. For controlling blood sugar, 500-700 mg of glucomannan per 100 calories in the diet has been used successfully in controlled research.
5. L-carnitine - L-carnitine is an amino acid needed to properly utilize fat for energy. When people with diabetes were given L-carnitine (1 mg per 2.2 pounds of body weight), high blood levels of fats (cholesterol and triglycerides) dropped 25 percent to 39 percent in just 10 days in one trial. L-carnitine also may help repair nerve damage in cases of diabetic neuropathy.
6. Bitter melon - Bitter melon's most notable benefit is in the area of diabetes treatment. Studies suggest the fruit may play a role in controlling the production of insulin by the body, thus promoting blood sugar control. Bitter melon was evaluated in 100 non-insulin-dependent diabetics for its impact on serum glucose levels. Eighty-six patients experienced a significant reduction of serum glucose levels following the ingestion of 200 mg of bitter melon, two times daily. The most current available medical and scientific literature indicates this dietary supplement should be standardized to 5.1% triterpenes.
Summary
Substantial evidence suggests type 2 diabetics respond most favorably to appropriate dietary and lifestyle modifications, as well as the use of targeted nutritional supplements. Too often, these proactive interventions are not addressed adequately in the global management of this condition. As such, chiropractors and other holistic practitioners should assess the patient's current lifestyle approach to his or her condition, and then be in a position to explain evidence-based complementary interventions that can improve type 2 diabetes and help prevent and manage the common complications of this disease.
Editor's note: To review the comprehensive list of resources/references for this article, please consult the online version: www.chiroweb.com/archives/23/20/30.html.
This article is available online at www.chiroweb.com/columnist/meschino. You may also leave a comment or ask a question at his "Talk Back" forum at the same location.
James Meschino, DC, MS. Previous articles, a "Talk Back" forum and a brief biography of the author are available online at www.chiroweb.com/columnist/meschino.
James Meschino, DC, MS
Toronto, Ontario
Canada
www.renaisante.com
Copyright Dynamic Chiropractic Sep 27, 2005
Provided by ProQuest Information and Learning Company. All rights Reserved