Several studies have suggested that there is a link between Reiter's syndrome and human immunodeficiency virus (HIV).(1-5) Based on this proposed link, the authors of those studies have recommended HIV testing in patients newly diagnosed for Reiter's syndrome. The purpose of this brief report is to review the current literature on HIV-positive Reiter's syndrome and to examine the recommendation for HIV testing of patients newly diagnosed for Reiter's syndrome. right achilles tendon. After a rheumatologist was consulted, the diagnosis of incomplete Reiter's syndrome was made. A radiograph of the pelvis revealed no evidence of sacroiliitis. The patient tested positive for HLAB27 and HIV antibody. The CD4 (helper) and CD8 (suppressor) cell counts were 126 and 801, respectively. The patient was advised to start zidovudine and trimethoprim-sulfamethoxazole. The arthritis subsided by the 5th month, at which time the patient was tapered off salicylates. Case Presentation A 32-year-old homosexual male patient presented to our office in November 1989 with complaints of watery, bloody diarrhea and fever, which had developed during a recent vacation in Mexico. The patient was treated with vibramycin, and his symptoms improved. When he was seen 3 weeks later, the patient had a 3-lb weight loss, bilateral conjunctivitis, neck stiffness, and effusions of both knees and one ankle. Arthrocentesis of the knee revealed an inflammatory fluid with neutrophil predominance but no crystals or bacteria. Gonococcal and bacterial cultures were negative, as were the serum rheumatoid factor, antinuclear antibodies, hepatitis panel, and Lyme disease titer. The sedimentation rate was greater than 150 mm/h. The rapid plasma reagin test was nonreactive. The electrocardiogram, obtained because of mildly elevated antistreptolysin and streptozyme titers, indicated only a wandering atrial pacemaker. An echocardiogram was normal. the patient was treated with oral erythromycin and high-dose salicylates for possible rheumatic fever; his symptoms abated.
During the 4th month after his initial presentation, the patient noted pain in his knees, ankles, right heel, and Discussion Reiter's syndrome has been defined in several ways. Classic Reiter's syndrome consists of the triad of asymmetric oligoarthritis, conjunctivitis, and nongonococcal urethritis or cervicitis.(6) The arthritis is inflammatory and usually affects one to five large joints of the lower extremities. Small joint or axial arthritis is sometimes seen. The conjunctivitis is generally transient and culture negative, and rarely requires therapy. The syndrome is heralded by urethritis/cervicitis or diarrhea. The urethritis or cervicitis, which may be sterile or grow chlamydia or ureaplasma, is thought to be sexually transmitted. The diarrhea may be culture negative or yield Salmonella, Shigella, Yersinia, Campylobacter(7,8) or possibly Giardia.(9,10) The diarrhea or cervicitis/urethritis usually precedes the onset of arthritis by 2 to 4 weeks.
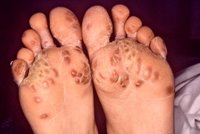
Patients with Reiter's syndrome may also have one or more of these associated symptoms: inflammation of the fingers or toes, inflammation of the tendinous attachment to bone, asymetric sacroiliitis, mucocutaneous lesions, or weight loss. The mucocutaneous lesions of Reiter's syndrome are keratoderma blennorrhagica, circinate balanitis, and painless oral ulcers. The lesions of keratoderma blennorrhagica are identical to pustular psoriasis. Patients with Reiter's syndrome have a high incidence of being HLA-B27 positive.(11) The HLA-B27 antigen has been associated with Reiter's syndrome in 63% to 96% of cases in white patients.(6) In the African population, however, where HLA-B27 prevalence is less than 1%, Reiter's syndrome has no apparent association with HLA-B27.(12)
Incomplete Reiter's syndrome was defined by Willkens and others(13) to be an episode of peripheral arthritis lasting 1 month or more, associated with urethritis or cervicitis. Calin (14) later defined incomplete Reiter's syndrome as an episode of peripheral arthritis lasting 1 month or more and associated with one or more other features seen in Reiter's syndrome. Patients are excluded if they have psoriatic arthritis or primary ankylosing spondylitis. (14,15)
The pathogenesis of Reiter's syndrome has not been elicited. In the white population, it is believed that there is a genetic predisposition (HLA-B27 positivity) and an environmental inducer (urethritis/cervicitis or dysentery). The above theory does not apply to the African population, with its negligible incidence of HLA-B27 positivity.
Reiter's syndrome, fairly rare in the general population, may be more prevalent in the HIV-positive population. In Rochester, Minnesota, Reiter's syndrome occurred in 0.006% of the population of 20- to 29-year-old men.(1,16) In studies of HIV-positive patients, higher prevalence rates were noted. Reiter's syndrome occurred in 0.3% of 2344 patients enrolled in the San Francisco AIDS registry (SFAR).(17,18) Calabrese,(19 Brancato and associates,(20) and Berman et al(3) examined patients for Reiter's syndrome in their HIV clinics and found prevalence rates of 4.2%,(19) 4.6%,(20,21) and 10%(3) out of 47, 65, and 101 consecutive patients, respectively. To date, 47 cases of Reiter's syndrome in HIV-positive patients have been reported.(2-4,12,19,20,22)
Immune dysfunction, cellular lymphokines, arthritogenic pathogens, and the direct effect of HIV have all been proposed as explanations for the possible association of HIV with Reiter's syndrome. Elevated ratios of CD8 to CD4, frequently seen in HIV infection, may induce Reiter's syndrome. The increase in CD8 cells is believed to be more important than the lack of CD4 cells, although the mechanism is unclear.(1,2,19) Another hypothesis is that HIV triggers an immune complex reaction.(3) Immune complexes have not been demonstrated in synovial membranes, however. Lymphokines have been linked to psoriatic arthritis' (3,23) and possibly to Reiter's syndrome. Arthritogenic pathogens such as Salmonella, Shigella, Yersinia, Campylobacter, and Giardia may be acquired in HIV-positive patients more readily than in HIV-negative patients owing to sexual practices.(1-3,20) Additionally, HIV-positive patients may harbor new arthritogenic bowel pathogens.(1) Finally, HIV may have a direct effect on synovial tissue. Using immunohistochemical methods, HIV antigens have been demonstrated in synovial fluid lymphocytes in HIV-associated reactive arthritis,(24) psoriatic arthritis, polymyositis, dermatomyositis, and vasculitis.(23) The importance of the latter finding is unknown.
One may wonder if the arthritis, conjunctivitis, and urethritis in these HIV-positive patients is Reiter's syndrome at aH. In three separate outpatient clinics for HIV-positive patients, Brancato and colleagues,(20) Calabrese,(19) and Berman and co-workers(3) reported arthritic complaint rates of 15%, 25%, and 68%, respectively. HIV-positive patients who arc sexually promiscuous have high rates of sexually transmitted diseases, and thus have urethritis or cervicitis frequently. The coincident occurrence of arthritis with urethritis may be mistakenly called incomplete Reiter's syndrome. However, these HIV-positive patients with Reiter's syndrome also had a high incidence of HLA-B27 positivity. The reported rates of HLA-B27 positivity in these HIV-positive patients with Reiter's syndrome were 63% by Berman et al,(3) 73% by Kaye,(1) and 75% by Winchester et al.(2) There does therefore seem to be true Reiter's syndrome in these HIV-positive individuals.
Conclusions about the prevalence of Reiter's syndrome in HIV-positive patients are difficult to make. The populations in Rochester, Minnesota,(16) and San Francisco(17) were far removed geographically. In addition, the Minnesota population was predominantly nonhomosexual in contrast to the California population. The age distribution of the SFAR series was not listed in the abstract, making statistical comparisons limited. The data from HIV clinics(3,19,20) were collected by unblinded physicians, thus introducing observer bias. Additionally, the series are small and contain no comparison groups. Further description and analysis of the data would provide useful information.
HIV-positive patients with Reiter's syndrome may be treated with nonsteroidal anti-inflammatory drugs (NSAIDs), analgesics, sulfasalazine,[sup. 2] or prednisone. Espinoza,(23) Brancato,(20) and Winchester(2) and their coworkers, as well as others, reported that NSAIDs and analgesics were variably effective. Espinoza et al(23) and Winchester et al(2) have also used prednisone with little benefit. On the other hand, the antimetabolite immunosuppressive medications used by Winchester(2) in HIV positive patients with Reiter's syndrome were associated with adverse consequences; two patients treated with methotrexate developed Pneumocystis carinii pneumonia and Kaposi's sarcoma, and one treated with azathiaprine developed severe, but reversible, fatigue and weight loss.(2)
Patients with HIV-positive Reiter's syndrome may have a more rapid course of their rheumatologic disease than HIV-negative Reiter's syndrome patients. In eight patients with Reiter's syndrome followed by Arnett an colleagues(6) in the 1970s, the duration of inflammatory arthropathy lasted from 8 months to 8 years. Ford25 states that the arthropathy, foot pain, and back pain may last several months. Winchester ct al(2) described 13 HIV-positive Reiter's syndrome patients. Five patients had aggressive joint destruction, and 8 had milder, recurrent episodes of arthritis about every 6 months. The more progressive arthritis was unresponsive to NSAIDs. The true course of the milder HIV-positive arthritis may be hard to assess because of the death of 9 of the 13 patients from AIDS.(2)
The clinical course of Reiter's syndrome in HIV-positive patients may be better studied in the future, now that patients with HIV disease are living longer with the use of prophylactic medications. Currently, the physician who sees a patient with urethritis or dysentery followed by arthritis should consider HIV infection, search for HIV risk factors, and propose HIV testing if indicated. Conclusions Relier's syndrome has been reported in HIV-positive patients. the data on HIV-positive Reiter's syndrome patients do not demonstrate a conclusive increase in prevalence in the HIV-positivc population compared with the HIV-negative population. Further data analysis and case-control studies will be needed to demonstrate this. Until it can be shown that Reiter's syndrome is more prevalent in the HIV-positive population, compared with the HIV-negative population, the HIV testing of all newly diagnosed Reiter's syndrome patients cannot be conclusively recommended. The physician would be prudent, however, to assess the HIV risk factors in Reiter's syndrome patients, since patients with Reiter's syndrome may have behaviors placing them at high risk for HIV infection.(26)
Key words: Reiter's disease; HIV; arthritis. Acknowledgements The authors wish to acknowledge Drs E. Sullivan, R. Winter, and A.
Picciano for their helpful comments on the manuscript. We would
like to thank Lena Freidel for her help in obtaining the necessary
references. References 1. Kaye BR. Rheumatologic manifestations of infection with human
immunodeficiency virus (HIV). Ann Intern Med 1989; 111:158 - 67. 2. Winchester R, Bernstein DH, Fischer HD, et al. The
co-occurrence of Reiter's syndrome and acquired immunodeficiency. Ann
Intern Med 1987-, 106:19-26. 3. Berman A, Espinoza LR, Diaz JD, et al. Pheumatic manifestations
of human immunodeficiency virus infection. Am j Med 1988;
85:59-64. 4. Forster SM, Siefert MH, Keat AC, et al. Inflammatory joint
disease and human immunodeficiency virus infection. Br Med J
1988; 296:1625-7. 5. Keat AC. Should all patients with Reiter's syndrome be tested for
HIV infection? Br j Rheumatol 1989; 28:409. 6. Arnett FC, McClusky OE, Schacter BZ, Lordon PE. Incomplete
Reiter's syndrome: discriminating features and HL-A W27 in
diagnosis. Ann Intern Med 1976; 84:8-12. 7. Keat A. Reiter's syndrome and reactive arthritis in perspective.
New Engl J Med 1983; 309:1606-15. 8. Vaughan J. Infection and rheumatic diseases: a review. Bull
Rheum Dis 1989; 39(l):5-6. 9. Shaw RA, Stevens MB. The reactive arthritis of giardiasis: a case
report. JAMA 1987; 258:2734-5. 10. Brancato LJ, Itescu S, Winchester R. Reiter's syndrome and related
rheumatic conditions in HIV infection. j Musculoskeletal
Med 1989; 15-32. 11. Brancato LJ, Calabrese LH, Chapman SW. Rheumatologic clues
to the STDS. Patient Care 1990; 24(14):79-103. 12. Davis P, Stein M, Latif A, Emmanuel J. Acute arthritis in Zimbabwean
patients: possible relationship to human immunodeficiency
virus infection. J Rheumatol 1989; 16:346-8. 13. Willkens PF, Arnett FC, Bitter T, et al. Reiter's syndrome: evaluation
of preliminary criteria for definite disease. Arthritis Rheum
1981; 24:844-9. 14. Calin A. Reiter's syndrome. In: Kelly WN, Harris E, Ruddy S,
Sledge C, eds. Textbook of rheumatology. Philadelphia: WB Saunders
Co, 1985:1007-20. 15. Calabro JJ. The seronegative spondyloarthropathies. A graduated
approach to management. Postgrad Med 1986; 80:173-88. 16. Michet CJ, Machado EB, Ballard Dj, McKenna CH. Epidemiology
of Reiter's syndrome in Rochester, Minnesota: 1950-1980.
Arthritis Rheum 1988; 31:428-31. 17. Clark M, Kinsolving M, Chernhoff D. The prevalence of arthritis
in two HIV-infected cohorts. Arthritis Rheum 1989; 32:S85. 18. Stein M, Davis P. HIV and arthritis-causal or casual acquaintances?
[Editorial]. J Rheumatol 1989; 16:1287-90. 19. Calabrese LH. The Rheumatic manifestations of infection with the
human immunodeficiency virus. Semin Arthritis Rheum 1989;
18:225-39. 20. Brancato L, Itescu S, Skovron ML, Solomon G, Winchester R.
Aspects of the spectrum, prevalence and disease susceptibility
determinants of Reiter's syndrome and related disorders associated
with HIV infection. Rheumatol Int 1989; 9:137-41. 21. Winchester R, Brancato L, Itescu S, Skovron ML, Solomon G.
Implications from the occurrence of Reiter's syndrome and related
disorders in association with advanced HIV infection. Scand J
Rheumatol Suppl 1988; 74:89-93. 22. Duvic M, Johnson TM, Rapini RP, Freese T, Brewton G, Rios A.
Acquired immunodeficiency syndrome-associated psoriasis and
Reiter's syndrome. Arch Dermatol 1987; 123:1622-32. 23. Espinoza LR, Aguilar JL, Berman A, Gutierrce F, Vasey FB,
Germain BF. Rheumatic manifestations associated with human
immunodeficiency virus infection. Arthritis Rheum 1989; 32:
1615-22. 24. Withrington RH, Comes P, Harris JRW, et al. Isolation of human
immunodeficiency virus from synovial fluid of a patient with
reactive arthritis. Br Med J 1987; 294:484. 25. Ford DK. Reiter's syndrome: reactive arthritis. In: McCarthy DJ,
cd. Arthritis and allied conditions. A textbook of rheumatology.
Philadelphia: Lea & Febiger 1989:944-53. 26. Winchester R. AIDS and the rheumatic diseases. Bull Rheum Dis
1990; 39(5):3-5. Submitted, revised, May 14, 1991. From the Family Practice Center, Jobn F. Kennedy Medical Center, Edison, New Jersey, and Sussex Family Practice Associates, Sussex, New Jersey. Requests for reprints should be addressed to Orlando F. Mills, MD, JFK Family Practice Center, 65 james St, Edison, NJ 08818. [C] 1991 Appleton & Lange ISSN 0094-3509
COPYRIGHT 1991 Dowden Health Media, Inc.
COPYRIGHT 2004 Gale Group