Rocky Mountain Spotted Fever and Human Ehrlichiosis - United States, 1989
Rocky Mountain Spotted Fever
In 1989, state health departments reported 603 cases of Rocky Mountain spotted fever (RMSF) to CDC, a 2.0% decrease from the 615 cases reported in 1988. The incidence rate was 0.25 per 100,000 persons. Of the 603 cases, 224 (37.1%) were reported from the South Atlantic region and 100 (16.6%) from the West South Central region. Oklahoma had the highest rate (62 cases, 1.9 per 100,000); other states with high rates were North Carolina (118 cases, 1.8 per 100,000), Montana (14 cases, 1.8 per 100,000), South Carolina (40 cases, 1.1 per 100,000), and Missouri (53 cases, 1.0 per 100,000) (Figure 1).
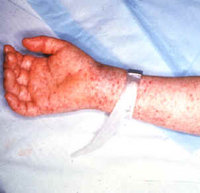
Detailed case reports were submitted on 487 (80.8%) cases. Of these, 300 (61.6%) were laboratory-confirmed,(*) 15 (3.1%) were classified as probable,(+) and 172 (35.3%) were not confirmed. Of the 487 cases, males accounted for 63.1% of cases. For 78.3% of cases, onset of symptoms occurred between May 1 and August 31 (with 46.8% of cases occurring in May and June); for 58.3%, a tick exposure within 14 days of symptoms was reported. Predominant manifestations included fever (90.4% of cases), headache (88.7%), myalgia (82.8%), rash (77.9%), and rash on palms (50.0%). The triad of fever, headache, and rash was present in 49.1% of cases. Age-specific incidence rates were highest in children aged 5-9 years (0.35 per 100,000) and lowest in persons aged 20-29 years (0.15 per 100,000) (Figure 2). The overall case-fatality rate was 1.2%. For persons [greater than or equal] 20 years of age, the case-fatality rate was 1.5%; for persons [less than] 20 years of age, the rate was 0.6%.
Although the total number of RMSF cases reported in 1989 decreased slightly from 1988, large increases in the number of cases occurred in two Mid-Atlantic states: New Jersey (from none in 1988 to 26 cases in 1989) and Pennsylvania (from two cases to 23 cases). A large decrease occurred in Kansas (26 cases in 1988 to 11 cases in 1989). The reasons for these fluctuations are unknown.
Human Ehrlichiosis
Ehrlichia is a genus in the family Rickettsiaceae; members of the genus are characterized by their parasitism of white blood cells. In 1986, human illness (ehrlichiosis) caused by an Ehrlichia (E. canis or a closely related species) was first recognized in the United States. Like RMSF, the disease appears to be transmitted by ticks and presents as an acute febrile illness (fever often exceeds 39 C [102.2 F]). Other common symptoms of ehrlichiosis and RMSF include myalgia, headache, and nausea and other gastrointestinal symptoms. Unlike RMSF, however, rash is usually fleeting and occurs in approximately one third of ehrlichiosis cases. About half of the patients have mild leukopenia, thrombocytopenia, and elevation of the alanine aminotransferase and aspartate aminotransferase.
Although no formal surveillance system exists for human ehrlichiosis, in 1989, 38 cases were detected by informal laboratory-based surveillance.([section]) Ten states had confirmed cases of human ehrlichiosis: Missouri (14 cases), Virginia (10), Oklahoma (four), Georgia (two), Tennessee (two), Washington (two), Arkansas (one), Illinois (one), Louisiana (one), and Texas (one). No fatal cases of human ehrlichiosis were reported for 1989.
Reported by: State health departments. Viral and Rickettsial Zoonoses Br, Div of Viral and Rickettsial Diseases, Center for Infectious Diseases, CDC. Editorial Note: During the 1980s, reported cases of RMSF declined from a high of 1170 cases in 1981 (1) to 592 cases in 1987 (2); small fluctuations in the number of cases have occurred since then. North Carolina led the nation in reported number of cases each year during the decade (mean: 179 per year), but Oklahoma had the highest incidence rate during 7 of the 10 years (mean: 3.1 per 100,000). Cases reported in males during the 1980s consistently exceeded those in females by a 3:2 ratio. The case-fatality rate was highest in 1982 (4.7%) (3) and lowest in 1989 (1.1%).
Because no laboratory test is consistently positive during the first 2 weeks of illness, patients with suspected RMSF should be treated empirically and serologic tests delayed until both acute and convalescent serum specimens are available. The indirect fluorescent antibody (IFA) and the indirect hemagglutination (IHA) tests are the most sensitive and specific of these tests (4,5). Complement-fixation, latex agglutination, and microagglutination are specific but lack the sensitivity of the IFA and IHA tests; negative results in one of these tests does not exclude the diagnosis of RMSF (4,5). The Weil-Felix test should not be used because it lacks both sensitivity and specificity. When paired serum specimens are not available, single specimens can be tested, but results may not be positive during the first 2 weeks of illness.
When diagnosis is considered essential to proper case management during the first 2 weeks of illness, a number of rapid diagnostic tests can be considered. Most untreated RMSF patients have rickettsemia; however, to determine the presence of rickettsiae, testing should be performed in only a few reference laboratories since laboratory-acquired infections have been reported (6). If a rash is present, a definitive diagnosis can sometimes be made by detecting Rickettsia rickettsii antigen in skin lesions, using a direct fluorescent antibody technique (7). However, the availability of this test is limited, and its sensitivity is only about 50%-70%. Recently, polymerase chain reaction technology was applied to the detection of R. rickettsii in the blood of a group of patients during the acute phase of infection (8).
Although substantially fewer cases of human ehrlichiosis than RMSF are reported, two recent studies indicate that in some geographic areas the incidence of human ehrlichiosis may equal or exceed that of RMSF. Of 249 paired serum samples submitted to the Oklahoma State Department of Health for RMSF testing in 1987, 29 (11.6%) were positive for antibody to E. canis and 29 (11.6%) were positive for R. rickettsii (9). Hospital-based active surveillance for human ehrlichiosis in southeast Georgia for an 18-month period in 1987 and 1988 detected eight cases, an annual rate of 5.3 per 100,000; during the same period, one case of RMSF was detected in this area (10).
Because no vaccine exists for RMSF, the best preventive measure is avoidance of tick-infested areas. Persons who must enter these areas should wear protective clothing. Attached ticks should be removed by grasping them with fine tweezers at the point of attachment and pulling gently (11). When fingers are used instead of tweezers, they should be protected with facial tissue and washed afterwards.
The polymerase chain reaction diagnostic test for RMSF and serologic tests for human ehrlichiosis are available for selected patients following consultation with state health departments or CDC's Viral and Rickettsial Zoonoses Branch, Division of Viral and Rickettsial Diseases, Center for Infectious Diseases (telephone [404] 639-1075). RMSF cases should be reported to state health departments.
References
[ 1.] CDC. Rocky Mountain spotted fever - United States, 1980. MMWR 1981;30:318-20. [ 2.] CDC. Rocky Mountain spotted fever - United States, 1987. MMWR 1988;37:388-9. [ 3.] CDC. Rocky Mountain spotted fever - United States, 1983. MMWR 1984;33:188-90, 195. [ 4.] Kaplan JE, Schonberger LB. The sensitivity of various serologic tests in the diagnosis of
Rocky Mountain spotted fever. Am J Trop Med Hyg 1986;35:840-4. [ 5.] Walker DH. Rocky Mountain spotted fever: a disease in need of microbiological concern. Clin
Microbiol Rev 1989;2:227-40. [ 6.] Pike RM. Laboratory-associated infections: summary and analysis of 3921 cases. Health Lab
Sci 1976;13:105-14. [ 7.] Walker DH, Cain BG. A method for specific diagnosis of Rocky Mountain spotted fever on
fixed, paraffin-embedded tissue by immunofluorescence. J Infect Dis 1978;137:206-9. [ 8.] Tzianabos T, Anderson BE, McDade JE. Detection of Rickettsia rickettsii DNA in clinical
specimens by using polymerase chain reaction technology. J Clin Microbiol 1989;27:
2866-8. [ 9.] Harkess JR, Ewing SA, Crutcher JM, Kudlac J, McKee G, Istre GR. Human ehrlichiosis in
Oklahoma. J Infect Dis 1989;159:576-9. [10.] Fishbein DB, Kemp A, Dawson JE, Greene NR, Redus MA, Fields DH. Human ehrlichiosis:
prospective active surveillance in febrile hospitalized patients. J Infect Dis 1989;160:803-9. [11.] Needham GR. Evaluation of five popular methods for tick removal. Pediatrics 1985;
75:997-1002. (*)A case is considered serologically confirmed if testing reveals an indirect fluorescent antibody (IFA) titer of [greater than or equal] 1:64, a complement-fixation (CF) titer of [greater than or equal] 1:16, or a fourfold rise in titer by the CF, IFA, microagglutination (MA), latex agglutination (LA), or indirect hemagglutination (IHA) tests. (+)A case is considered probable if testing reveals a fourfold rise in titer or a single titer [greater than or equal] 1:320 in the Weil-Felix test or an IFA, LA, or MA single titer of [greater than or equal] 1:128. ([section])A case is considered serologically confirmed if testing reveals a fourfold rise or fall in antibody titer, with a titer of at least 1:64, in an IFA to E. canis.
COPYRIGHT 1990 U.S. Government Printing Office
COPYRIGHT 2004 Gale Group