Definition
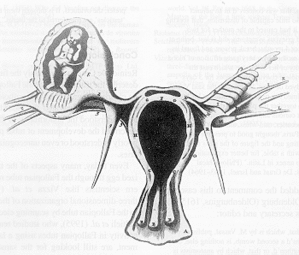
In an ectopic pregnancy, the fertilized egg implants in a location outside the uterus and tries to develop there. The word ectopic means "in an abnormal place or position." The most common site is the fallopian tube, the tube that normally carries eggs from the ovary to the uterus. However, ectopic pregnancy can also occur in the ovary, the abdomen, and the cervical canal (the opening from the uterus to the vaginal canal). The phrases tubal pregnancy, ovarian pregnancy, cervical pregnancy, and abdominal pregnancy refer to the specific area of an ectopic pregnancy.
Description
Once a month, an egg is produced in a woman's ovary and travels down the fallopian tube where it meets the male's sperm and is fertilized. In a normal pregnancy the fertilized egg, or zygote, continues on its passage down the fallopian tube and enters the uterus in three to five days. The zygote continues to grow, implanting itself securely in the wall of the uterus. The zygote's cells develop into the embryo (the organism in its first two months of development) and placenta (a spongy structure that lines the uterus and nourishes the developing organism).
In a tubal ectopic pregnancy, the fertilized egg cannot make it all the way down the tube because of scarring or obstruction. The fallopian tube is too narrow for the growing zygote. Eventually the thin walls of the tube stretch and may burst (rupture), resulting in severe bleeding and possibly the death of the mother. More than 95% percent of all ectopic pregnancies occur in the fallopian tube. Only 1.5% develop in the abdomen; less than 1% develop in the ovary or the cervix.
Causes & symptoms
As many as 50% of women with ectopic pregnancies have a history of pelvic inflammatory disease (PID). This is an infection of the fallopian tubes (salpingitis) that can spread to the uterus or ovaries. It is most commonly caused by the organisms Gonorrhea and Chlamydia and is usually transmitted by sexual intercourse.
Other conditions also increase the risk of ectopic pregnancy. They include:
- Endometriosis. A condition in which the tissue that normally lines the uterus is found outside the uterus, and can block a fallopian tube.
- Exposure to diethylsilbestrol (DES) as a fetus. If a woman's mother took DES (a synthetic version of the hormone estrogen) during pregnancy, the woman may have abnormalities in her fallopian tubes that can make ectopic pregnancy more likely.
- Taking hormones. Estrogen and progesterone are hormones that regulate the menstrual cycle and may be in medications prescribed by a doctor for birth control or other reasons. Taking these hormones can affect the interior lining of the fallopian tubes and slow the movement of the fertilized egg down the tube. Women who become pregnant in spite of taking some progesterone-only contraceptives have a greater chance of an ectopic pregnancy. Ectopic pregnancy is also more likely when the ovaries are artificially stimulated with hormones to produce eggs for in vitro fertilization (a procedure in which eggs are taken from a woman's body, fertilized, and then placed in the uterus in an attempt to conceive a child).
- Use of an intrauterine device (IUD). These contraceptive devices are designed to prevent fertilized eggs from becoming implanted in the uterus, but they have only a minimal effect on preventing ectopic pregnancies. Therefore, if a woman becomes pregnant while using an IUD for contraception, the fertilized egg is more likely to be implanted someplace other than the uterus. For example, among women who become pregnant while using a progesterone-bearing IUD, about 15% have ectopic pregnancies.
- Surgery on a fallopian tube. The risk of ectopic pregnancy can be as high as 60% after undergoing elective tubal sterilization, a procedure in which the fallopian tubes are severed to prevent pregnancy. Women who have successful surgery to reverse the procedure are also more likely to have an ectopic pregnancy.
Early symptoms
In an ectopic pregnancy all the hormonal changes associated with a normal pregnancy may occur. The early symptoms include: fatigue; nausea; a missed period; breast tenderness; low back pain; mild cramping on one side of the pelvis; abnormal vaginal bleeding, usually spotting.
Later symptoms
As the embryo grows too large for the confined space in the tube, the first sign that something is wrong may be a stabbing pain in the pelvis or abdomen. If the tube has ruptured, blood may irritate the diaphragm and cause shoulder pain. Other warning signs are lightheadedness and fainting.
Diagnosis
To confirm an early diagnosis of ectopic pregnancy, the doctor must determine first that the patient is pregnant and that the location of the embryo is outside the uterus. If an ectopic pregnancy is suspected, the doctor will perform a pelvic examination to locate the source of pain and to detect a mass in the abdomen.
Several laboratory tests of the patient's blood provide information for diagnosis. Measurement of the human chorionic gonadotropin (hCG) level in the patient's blood serum is the most useful laboratory test in the early stages. In a normal pregnancy, the level of this hormone doubles about every two days during the first ten weeks. In an ectopic pregnancy, the rate of the increase is much slower and the low hCG for the stage of the pregnancy is a strong indication that the pregnancy is abnormal. (It could also represent a miscarriage in progress.) The level is usually tested several times over a period of days to determine whether or not it is increasing at a normal rate.
Progesterone levels in the blood are also measured. Lower than expected levels can indicate that the pregnancy is not normal.
An ultrasound examination may provide information about whether or not the pregnancy is ectopic. A device called a transducer, which emits high frequency sound waves, is moved over the surface of the patient's abdomen or inserted into the vagina. The sound waves bounce off of the internal organs and create an image on a screen. The doctor should be able to see whether or not there is a fetus developing in the uterus after at least five weeks of gestation. Before that point, a normal pregnancy is too small to see.
A culdocentesis may also help confirm a diagnosis. In this procedure a needle is inserted into the space at the top of the vagina, behind the uterus and in front of the rectum. Blood in this area may indicate bleeding from a ruptured fallopian tube.
A laparoscopy will enable the doctor to see the patient's reproductive organs and examine an ectopic pregnancy. In this technique, a hollow tube with a light on one end is inserted through a small incision in the abdomen. Through this instrument the internal organs can be observed.
Treatment
Ectopic pregnancy requires immediate treatment. The earlier the condition is treated, the better the chance to preserve the fallopian tube intact for future normal pregnancies.
Medical
If the ectopic pregnancy is discovered in a very early stage of development, the drug methotrexate may be given. The best results are obtained when the pregnancy is less than six weeks old and the tubal mass is no more than 1.4 in (3.5 cm) in diameter. Methotrexate, which has been used successfully since 1987, works by inhibiting the growth of rapidly growing cells. (It is also used to treat some cancers.) Most side effects are mild and temporary, but the patient must be monitored after treatment. Usually the medication is injected into the muscle in a single dose, but may also be given intravenously or injected directly into the fallopian tube to dissolve the embryonic tissue. Methotrexate has also been used to treat ovarian, abdominal, and cervical pregnancies that are discovered in the early stages.
Surgical
When a laparoscopy is done to visualize the ectopic pregnancy, the scope can be fitted with surgical tools and used to remove the ectopic mass immediately after it is identified. The affected fallopian tube can be repaired or removed as necessary. This procedure can be done without requiring the patient to stay in the hospital overnight.
When the pregnancy has ruptured, a surgical incision into the abdomen, or laparotomy, is performed to stop the immediate loss of blood and to remove the embryo. This usually requires general anesthesia and a hospital stay. Every effort is made to preserve and repair the injured fallopian tube. However, if the fallopian tube has already ruptured, repair is extremely difficult and the tube is usually removed.
Alternative treatment
Ectopic pregnancy was first described in the eleventh century and was a potentially fatal condition until the advent of surgery and blood transfusions in the early twentieth century. The sophisticated diagnostic tools and surgical procedures developed since the 1970s have equipped modern medicine with the tools to not only save a woman's life, but also to preserve her future fertility.
Although there are herbal remedies for the temporary relief of the common symptoms of anxiety and abdominal discomfort, prompt medical treatment is the only sure remedy for ectopic pregnancy.
Prognosis
Ectopic pregnancies are the leading cause of pregnancy-related deaths in the first trimester and account for 9% of all pregnancy-related deaths in the United States. More than 1% of pregnancies are ectopic and they are becoming more common. The reason for this increase is not clearly understood, though it is thought that the dramatic increase in sexually transmitted diseases (STD) is at least partly responsible.
The earlier an ectopic pregnancy is diagnosed and treated, the better the outcome. The chances of having a successful pregnancy are lower after an ectopic pregnancy, but depend on the extent of permanent fallopian tube damage. If the tube has been spared, chances are as high as 60%. The chances of a successful pregnancy after the removal of one tube are 40%.
Prevention
Many forms of ectopic pregnancy cannot be prevented. However, tubal pregnancies, which make up the majority of ectopic pregnancies, may be prevented by avoiding conditions that cause damage to the fallopian tubes. Since half of all women who experience ectopic pregnancy have a history of PID, avoiding this infection or getting early diagnosis and treatment for sexually transmitted diseases will decrease the risk of a future problem.
Key Terms
- Embryo
- In humans, the developing organism from conception until approximately the end of the second month.
- Fallopian tube
- The tube that carries the egg from the ovary to the uterus.
- Human chorionic gonadotropin (hCG)
- A hormone excreted during the development of an embryo or fetus.
- Laparoscopy
- Examination of the contents of the abdominal cavity with a fiberoptic tube inserted through a small incision.
- Laparotomy
- Surgical incision into the abdomen to locate, repair, and/or remove injured or diseased tissues.
- Pelvic inflammatory disease (PID)
- Acute or chronic inflammation in the pelvic cavity, particularly inflammation of the fallopian tubes (salpingitis) and its complications.
- Rupture
- A breaking apart of an organ or tissue.
- Salpingitis
- Inflammation of the fallopian tube.
- Tubal pregnancy
- Pregnancy in one of the fallopian tubes.
- Zygote
- The fertilized egg.
Further Reading
For Your Information
Books
- Cunningham, F. Gary, et al. "Ectopic Pregnancy." In Williams Obstetrics. Appleton & Lange, 1997. pp. 607-629.
- Stabile, Isabel. Ectopic Pregnancy: Diagnosis and Management. Cambridge University Press, 1996.
Periodicals
- Maiolatesi, C. R. "Methotrexate for Nonsurgical Treatment of Ectopic Pregnancy: Nursing Implications." Journal of Obstetrical Gynecological Neonatal Nursing (March/April 1996):205-208.
Organizations
- Resolve. 1310 Broadway, Somerville, MA 02144-1731. (617) 623-0477. http:///www.resolve.org.
Gale Encyclopedia of Medicine. Gale Research, 1999.