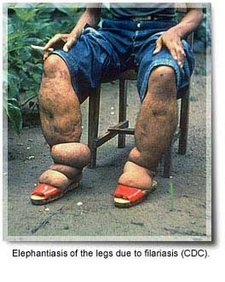
Definition
Filiariasis is the name for a group of tropical diseases caused by various thread-like parasitic round worms (nematodes) and their larvae. The larvae transmit the disease to humans through a mosquito bite. Filariasis is characterized by fever, chills, headache, and skin lesions in the early stages and, if untreated, can progress to include gross enlargement of the limbs and genitalia in a condition called elephantiasis.
Description
Approximately 170 million people in the tropical and subtropical areas of southeast Asia, South America, Africa, and the islands of the Pacific are affected by this debilitating parasitic disease. While filariasis is rarely fatal, it is the second leading cause of permanent and long-term disability in the world. The World Health Organization (WHO) has named filariasis one of only six "potentially eradicable" infectious diseases and has embarked upon a 20-year campaign to eradicate the disease.
In all cases, a mosquito first bites an infected individual then bites another uninfected individual, transferring some of the worm larvae to the new host. Once within the body, the larvae migrate to a particular part of the body and mature to adult worms. Filariasis is classified into three distinct types according to the part of the body that becomes infected: lymphatic filariasis affects the circulatory system that moves tissue fluid and immune cells (lymphatic system); subcutaneous filariasis infects the areas beneath the skin and whites of the eye; and serous cavity filariasis infects body cavities but does not cause disease. Several different types of worms can be responsible for each type of filariasis, but the most common species include the following: Wucheria bancrofti, Brugia malayi (lymphatic filariasis), Onchocerca volvulus, Loa loa, Mansonella streptocerca, Dracunculus medinensis (subcutaneous filariasis), Mansonella pustans, and Mansonella ozzardi (serous cavity filariasis).
The two most common types of the disease are Bancroftian and Malayan filariasis, both forms of lymphatic filariasis. The Bancroftian variety is found throughout Africa, southern and southeastern Asia, the Pacific islands, and the tropical and subtropical regions of South America and the Caribbean. Malayan filariasis occurs only in southern and southeastern Asia. Filariasis is occasionally found in the United States, especially among immigrants from the Caribbean and Pacific islands.
A larvae matures into an adult worm within six months to one year and can live between four and six years. Each female worm can produce millions of larvae, and these larvae only appear in the bloodstream at night, when they may be transmitted, via an insect bite, to another host. A single bite is usually not enough to acquire an infection, therefore, short-term travelers are usually safe. A series of multiple bites over a period of time is required to establish an infection. As a result, those individuals who are regularly active outdoors at night and those who spend more time in remote jungle areas are at an increased risk of contracting the filariasis infection.
Causes and symptoms
In cases of lymphatic filariasis, the most common form of the disease, the disease is caused by the adult worms actually living in the lymphatic vessels near the lymph nodes where they distort the vessels and cause local inflammation. In advanced stages, the worms can actually obstruct the vessels, causing the surrounding tissue to become enlarged. In Bancroftian filariasis, the legs and genitals are most often involved, while the Malayan variety affects the legs below the knees. Repeated episodes of inflammation lead to blockages of the lymphatic system, especially in the genitals and legs. This causes the affected area to become grossly enlarged, with thickened, coarse skin, leading to a condition called elephantiasis.
In conjunctiva filariasis, the worms larvae migrate to the eye and can sometimes be seen moving beneath the skin or beneath the white part of the eye (conjunctiva). If untreated, this disease can cause a type of blindness known as onchocerciasis.
Symptoms vary, depending on what type of parasitic worm has caused the infection, but all infections usually begin with chills, headache, and fever between three months and one year after the insect bite. There may also be swelling, redness, and pain in the arms, legs, or scrotum. Areas of pus (abscesses) may appear as a result of dying worms or a secondary bacterial infection.
Diagnosis
The disease is diagnosed by taking a patient history, performing a physical examination, and by screening blood specimens for specific proteins produced by the immune system in response to this infection (antibodies). Early diagnosis may be difficult because, in the first stages, the disease mimics other bacterial skin infections. To make an accurate diagnosis, the physician looks for a pattern of inflammation and signs of lymphatic obstruction, together with the patient's possible exposure to filariasis in an area where filariasis is common. The larvae (microfilariae) can also be found in the blood, but because mosquitos, which spread the disease, are active at night, the larvae are usually only found in the blood between about 10 pm and 2 am.
Treatment
Either ivermectin, albendazole, or diethylcarbamazine is used to treat a filariasis infection by eliminating the larvae, impairing the adult worms' ability to reproduce, and by actually killing adult worms. Unfortunately, much of the tissue damage may not be reversible. The medication is started at low doses to prevent reactions caused by large numbers of dying parasites.
While effective, the medications can cause severe side effects in up to 70% of patients as a result either of the drug itself or the massive death of parasites in the blood. Diethylcarbamazine, for example, can cause severe allergic reactions and the formation of pus-filled sores (abscesses). These side effects can be controlled using antihistamines and anti-inflammatory drugs (corticosteroids). Rarely, treatment with diethylcarbamazine in someone with very high levels of parasite infection may lead to a fatal inflammation of the brain (encephalitis). In this case, the fever is followed by headache and confusion, then stupor and coma caused when massive numbers of larvae and parasites die. Other common drug reactions include dizziness, weakness, and nausea.
Symptoms caused by the death of the parasites include fever, headache, muscle pain, abdominal pain, nausea and vomiting, weakness, dizziness, lethargy, and asthma. Reactions usually begin within two days of starting treatment and may last between two and four days.
No treatment can reverse elephantiasis. Surgery may be used to remove surplus tissue and provide a way to drain the fluid around the damaged lymphatic vessels. Surgery may also be used to ease massive enlargement of the scrotum. Elephantiasis of the legs can also be helped by elevating the legs and providing support with elastic bandages.
Prognosis
The outlook is good in early or mild cases, especially if the patient can avoid being infected again. The disease is rarely fatal, and with continued WHO medical intervention, even gross elephantiasis is now becoming rare.
Prevention
The best method of preventing filariasis is to prevent being repeatedly bitten by the mosquitoes that carry the disease. Some methods of preventing insect bites include the following:
- Limit outdoor activities at night, particularly in rural or jungle areas.
- Wear long sleeves and pants and avoid dark-colored clothing that attracts mosquitoes.
- Avoid perfumes and colognes.
- Treat one or two sets of clothing ahead of time with permethrin (Duramon, Permanone).
- Wear DEET insect repellent or, especially for children, try citronella or lemon eucalyptus, to repel insects.
- If sleeping in an open area or in a room with poor screens, use a bed net to avoid being bitten while asleep.
- Use air conditioning. You will not have to open the doors and windows and the cooler air makes insects less active.
In addition, filariasis can be controlled in highly infested areas by taking ivermectin preventatively before being bitten. Currently, there is no vaccine available, but scientists are working on a preventative vaccine at this time.
Key Terms
- Abscess
- An area of inflamed and injured body tissue that fills with pus.
- Antibody
- A specific protein produced by the immune system in response to a specific foreign protein or particle called an antigen.
- Conjunctiva
- The mucous membrane that lines the inside of the eyelid and the exposed surface of the eyeball.
- Elephantiasis
- A condition characterized by the gross enlargement of limbs and/or the genitalia that is also accompanied by a hardening and stretching of the overlying skin. Often a result of an obstruction in the lymphatic system caused by infection with a filarial worm.
- Encephalitis
- Inflammation of the brain.
- Lymphatic system
- The circulatory system that drains and circulates fluid containing nutrients, waste products, and immune cells, from between cells, organs, and other tissue spaces.
- Microfilariae
- The larvae and infective form of filarial worms.
- Nematode
- Round worms.
- Subcutaneous
- The area directly beneath the skin.
Further Reading
For Your Information
Books
- Bannister, Barbara A., Norman T. Begg, and Stephen H. Gillespie. Infectious Disease. Oxford, England: Blackwell Scientific, Inc., 1996.
- Turkington, Carol A. Infectious Diseases A to Z. New York: Facts on File, Inc., 1998.
- Van De Graaff, Kent. Survey of Infectious and Parasitic Diseases. New York: McGraw Hill, 1996.
- Wilks, David, Mark Farrington, and David Rubenstein. The Infectious Diseases Manual. Oxford, England: Blackwell Scientific, Inc., 1995.
Periodicals
- Burnham, Gilbert M. "Ivermectin Where Loa Loa is Endemic." The Lancet. 349 (9070)(July 5, 1997):2-3.
- Cunningham, Nancy M. "Lymphatic Filariasis in Immigrants From Developing Countries." American Family Physician. 55 (4)(March 1997:1199-1204.
- WHO editors. "Lymphatic Filariasis: Diagnosis and Pathogenesis." Bulletin of the World Health Organization. 71 (2)(March-April 1993):135-41.
Organizations
- Centers for Disease Control. 1600 Clifton Rd., NE, Atlanta, GA 30333. (404) 639-3311. http://www.cdc.gov/travel/travel.html.
- National Institute of Allergies and Infectious Diseases, Division of Microbiology and Infectious Diseases. Bldg. 31, Rm. 7A-50, 31 Center Drive MSC 2520, Bethesda, MD 20892.
- World Health Organization, Division of Emerging and Other Communicable Diseases Surveillance and Control. 1211 Geneva 27, Switzerland. http://www.who.ch.
Other
- Bacterial Diseases (Healthtouch). http:www.healthtouch.com/level1/leaflets/105825/105826.htm.
- Bug Bytes. http:www.isumc.edu/bugbytes/.
- CDC editors. Lymphatic Filariasis. CDC web page. http://www.cdc.gov/travel/yellowbk/page117.htm.
- Emerging Infectious Diseases Journal, National Center for Infectious Diseases. http://www.cdc.gov/ncidod/EID/eidtext.htm.
- International Society of Travel Medicine. http:www.istm.org.
- Travel Health editors. Filariasis (Other Than Loa Loa and Onchocerciasis). Travel Health Information and Referral Service website (March 5, 1997). http://www.travelhealth.com.
Gale Encyclopedia of Medicine. Gale Research, 1999.