SUMMARY
Abdominal angiostrongyliasis is a zoonotic infection produced by a metastrongylid intra-arterial nematode, Angiostrongylus costaricensis. Human accidental infection may result in abdominal lesions and treatment with anti-helminthics is contra-indicated because of potential higher morbidity with excitement or death of worms inside vessels. To evaluate the effect of mebendazole on localization of the worms, male Swiss mice, 5 week-old, were infected with 10 third stage larvae per animal. Twelve infected mice were treated with oral mebendazol, at 5 mg/kg/day, for 5 consecutive days, begining 22 days after inoculation. As control groups, 12 infected but non-treated mice and other 12 non-infected and non-treated mice were studied. The findings at necropsy were, respectively for the treated (T) and control (C) groups: 92% and 80% of the worms were inside the cecal mesenteric arterial branch; 8% and 10% were located inside the aorta. Only in the group C some worms (10%) were found inside the portal vein or splenic artery. These data indicate that treatment with mebendazole does not lead to distal or ectopic migration of A. costaricensis worms.
KEYWORDS: Angiostrongylus costuricencis; Adult stage; Migration; Mebendazole.
INTRODUCTION
Angiosirongylus costaricensis (Ncmatoda: Angiostrongylidae), MORHRA & CESPEDBS 1971, is a ncmaiodc that lives inside the ileocolic branches of mesenteric artery is a wild rodents, like the cotton rat, Sigmodon hispidus. The parasite, its cycle and the disease were first described in Costa Rica (CESPBDES et al, 1967; MORERA, 1973). Man is an accidental host, that may become infected by ingestion of food or water contaminated with third stage larvae, which may be present in the mucous secretion of vcronicellid slugs, the most important intermediate host (MORERA, 1985).
The geographic range of the parasitosis includes most of the countries in the Americas, from the south of the United States to the north of Argentina (DEMO & PESSAT, 1986; MORERA, 1988). In Brazil, the occurrence of abdominal angiostrongyliasis has been reported since 1975 (ZILIOTTO et al., 1975). The worm causes in man an infection called abdominal angiostrongyliasis, a parasitic disease characterized by a granulomatous inflammatory reaction with heavy cosinophilic infiltration of intestinal wall, especially in the ilco-cccal region (MORERA, 1967; GRAEPP-TEIXElRA et al., 1991). Until now there is no effective medical treatment and there is even a relative contra-indication for the use of anti-helminthics, based on data reported by MORERA & RONTEMPO ( 1985) suggesting that parasites were excited by the drugs instead of killed, causing erratic migration and worsening of the lesions. After these, some drug trials have demonstrated a predominant larvicidal effect, but none of those experiments was concerned with the possibility of migration of the adult worm after treatment, as it is the case in the present study, with mcbcndazolc.
MATERIALS AND METHODS
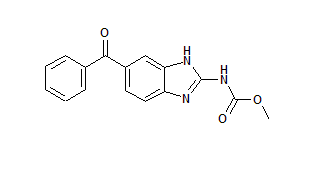
The infective third-stage Angiostrongylus costaricensis larvae (L3), Santa Rosa strain, were inoculated through a metal canula, into 6 week-old male Swiss mice (Mus domesticus domesticus). The larvae were obtained from experimentally infected Phyllocaulis soleiformis slugs. The molluscs were digested in a 0.03% pepsin (Sigma P-7125) solution in 0.7% HCl for 2 hours at 37 °C. Two groups (T and C) of 12 mice each, were inoculated with 10 L3 per animal. The first group (T), was treated with five successive doses of mebendazole (methyl 5-benzoyl-2-benzimidazole-carbamate) at 5 mg/kg/day, starting 22 days post-infection (dpi). Mebendazole (BYC, Dinamarc) was suspended in 100 pL of distilled water and given orally with a metal catheter. To both control groups, C (infected and non-treated) and N (non-infected and non-treated) only 100 µL of distilled water was administered per os.
The animals were kept on standard laboratory conditions with food and tap water ad libitum. In order to confirm the infection, after 21 dpi we started daily individual observation of the number of first larvae stage (Ll) in feces, for seven days, using the Bacrmann-Moraes modified method. all surviving mice were sacrificed by CO2 inhalation at 27 dpi and examined for the presence, number and location of adult worms.
RESULTS AND DISCUSSION
The results arc shown in the Table I. Both in treated and non-treated groups most of the worms were found in their usual location, the main branches of mcscntcric artery.
Efficacy of a chemotherapcutic treatment is influenced by various factors including route, dosage and regimen of the treatment. In addition, in the treatment of the diseases by tissue dwelling parasites, allcrgenic components of killed worms may cause adverse effects on the host (HAWKING, 1979; JOUBERT et al., 1985; HAYASHl, 1987). Therefore, effective treatment should only be establishcd after these factors arc taken into account through basic studies using experimental models.
In several experimental studies with Angiostrongylus spp, a number of parameters have been observed, like body weight, host death, relative spleen weight, pathologic changes on the scrosal surface of cccum and ileum, hematologie examination, larvae elimination in feces and eggs in intestinal wall, as well as the number of recovered worms, their body length and morphologic changes (TERADA et al., 1993). Study on the localization of worms as an effect of the drug has never been performed with abdominal angiostrongyliasis.
Recent studies about mode of action of mebcndaxole (methyl 5-bcnzoyl-2-bcnzimidazolc-carbamate) suggested interruption of microtubular function as its primary mechanism of action. It secondarily inhibits glucose uptake, fumarate redutase activity, egg hatching and larval development (REW & FETTERER, 1986). Killing effect is thought to result not only from drug action but also from the host's immune response as suggested initially by TERADA et; al. (1992).
TUNGTRONGCHITR ef al. (I993a) suggested that different mechanisms resulting in damage to the worms and to the host would be related to different regimens of mebendazolc. When host mice were treated successively with higher doses, worms would be killed abruptly due to anthelmintic action of mebendazolc, causing rather severe side effects. When mice were treated intermittently with lower doses, the worms were weakened by the anthelmintic and died more gradually through a combination of drug action and host defense, resulting in fewer side effects. A daily dose of 5 mg/Kg was selected because its efficacy and safety to treat murinc angioslrongyliasis in the adult stage was demonstrated by other authors (TERADA at al., 1993; TUNGTRONGCHITR et al., 1993a).
Treatment did not reduce the number of recovered worms: 36 in the mebendazole group and 30 in control group. This seems to confirm the idea that mebendazole is predominantly a larvicidal drug, with little killing effect at adult stages, as shown by TRRADA et al. (1992): the worm recovery decreased only with earlier administration, such as 1025 days p.i.
TUNGTRONGCHlTR et al. ( 1993b) showed thnt the treatment with mebendazole, even with some reduction in the number of worms, could not completely prevent host death, probably because of allergenic reactions to substances released by dead worms. In the present work, mortality was 83% in the non-treated infected control group (C group) and 67% in mebendazole treated group (T group). This difference in mortality can not be attributed to a killing effect on adult worms, since their number was not reduced, but may be linked to the reduction both in the number of animals with L1 elimination (C group: 62.5%; T group: 100%). It could be an effect of mebendazole on egg formation and/or oviposition, as previously suggested by THRADA et al. (1993). These authors demonstrated that mebendazole can completely abolish larval output, a result only partially now reproduced, with the same successive daily dosis.
In both groups, most of the worms were located in the main branches of mcscntcric artery: 24 (80%) and 33 (92%), respectively in control and treated groups (Table I ), in accordance with the data from TERADA ef a/. (1993). Only 8% of the worms in treated animals were found in the thoracic aorta, that should not be considered an cctopic location since one main route (lymphatic-arterial) for development of A. costaricensis includes the aorta (MOTA & LBNZI, 1995). Even if one considers it as cctopic location, it is not attributable to mebendazole, since 10% of worms in the control group were also in that location.
In conclusion, the data now reported docs not support the hypothesis that mebendazole induces cctopic migration of the A. costaricensis adult worms in the murine model.
RESUMO
O tratanicnto com mcbendazol nao esta associado a migracao distal de adultes de Angiostrongylus costaricensis na infeccao experimental murina
Angiostrongiliase abdominal e um a zoonose causada por um mctastrongilidco intra-arlerial, o Angiostrongylus costaricensis. Infeccao acidcntal humana pode rcsultar cm docnca abdominal c o iralamcnto com anti-helminticos c contra-indicado pela possibilidade de agravamento das lesoes coin a excitacao ou morte dos vermcs intravasculares. Para avaliar o efeito do mcbendazole sobre a localizacao dos vcrmes, camundongos Swiss machos, com 5 semanas de idade foram infcctados individualmcntc com 10 larvas de tcrceiro cstagio. Dozc dclcs foram tratados 22 dias apos a inl'eccao, corn mebendazole, na dose de 5 mg/kg/dia, por 5 dias consecutivos. Igual numero de camundongos inlcctados, nao tratados e um tercciro grupo de animais nao infectados e nao tratados, serviram como grupos controles. A necropsia observaramse os seguinles resultados: a proporcao de vermcs adultos encontrados na arteria mcsenterica do ceco c colon foi de 80% no grupo C e 92% no grupo T. A proporcao de vermcs adullos encontrados na aorta toracica foi de 10% no grupo C e de 8% no grupo T. No grupo C, 10% dos vermes tambcm foram encontrados na veia porta e na arteria esplcnica. Estes resultados indicam que o mebendazole nao induz migracao cctopica ou distal do Angioslrongylus costaricensis.
REFERENCES
1. CESPEDES, K.: SALAS, J.: MKKRIiL. S. et al. - Granulomas cmericos y linfaticos con intensn eosinofilin tisulnr proclucidos por un slrongilideo (slrongylata). Acta med. costarric., 10: 235-255, 1967.
2. DEMO. O.J. & PESSAT. O.A.N. - Angiostrongilosis abdominal, Primer caso humano encontraclo en Argentina. Prensa med. argent., 73: 732-738, 1986.
3. GRAEFF-TEIXEIRA, C.; CAMILLO-COURA, L. & LENZI, H.I. - Clinical and epidcmiological aspects of abdominal angiostrongyliasis in Southern Brazil. Rev. Inst. Mod. trop. S. Paulo. 33: 373-378, 1991.
4. HAWKING, E. - Diethylcarbaniiizine and new compounds for the treatment of filariasis. Aclvanc. Pharmacol. Chcmothcr., 16: 129-194, 1979.
5. HAYASHI, M. - Studies on chemotherapy of parasitic helminths. (XXX). Clinical and pathological changes in miccs infected with Angioslrongylus canlonensis and treatment wilh mebendazole and bctamethasone. Jap. J. Parasit., 36: 80-87, 1987.
6. JOUBERT, J.: JOUBRRT, M.J. & LOMBAARD. CM. - Neurocysticercosis: a comprehensive approach to medical treatment. S. Afr. med. J., 68: 11-14, 1985.
7. MORERA, P. - Granulomes entcricos y linfaticos con intensa cosinofilia tisular producidos por un c.strongilideo (Strongyiata: Raillet y Henry, 1913). II. Aspecto para.sitologico (Nota previa). Acta med. costarric., 10: 257-265, 1967.
8. MORlZRA, P. - Life history and rcdcscription of Angiostrongylus coslaricensis Morcra & Cespedes, 1971. Amcr. J. trop. Mcd. Hyg., 22: 613-621, 1973.
9. MORRRA, P. - Abdominal angiostrongyliasis; a problem of public health. Parasit, today, 1: 173-175, 1985.
10. MORERA, P. - Angiostrongilia.se abdominal. Um problcma de Saude Publica? Rev. Soc. bras. Mcd. trop., 21: 81-83, 1988.
11. MORF.RA, P. & BONTEMPO, I. - Accion de algunos antihelminticos sobre Aiigiiistmiigylux cnxtaricenxix. Rcv. mcd. Hosp. nac. Ninos Costa Rica, 20: 165-174, 1985.
12. MORERA, P. & CESPEDES, R. - Angiostrongilosis abdominal. Una nueva parasitosis humana. Acta mcd. costarric., 14: 159-173, 1971.
13. MOTA, E.M. & LENZI, H.L. - Angiostrongylus costaricensis life cycle. A new proposal. Mem. Inst. Oswaldo Cruz, 90: 707-709, 1995.
14. REW. R.S. & FETTERER, R.H. - Mode of action of antinematodal drugs. In: CAMPBELL, W.C. & REW, R.S.,ed. Chemotherapy of parasitic diseases. New York, Plenum Press, 1986. p. 321-337.
15. TERADA, M.; KINO, H.; AKYOL, C.V. & SANO, M. - Effects of mebendazole on Angiostrongylus costaricensis in mice with special reference to the timing of treatment. Parasit. Res., 79: 441-443, 1993.
16. TERADA, M.; TUNGTRONGCHITR, A.; ISHII, A. & SANO, M. - Effects of mebendazole on abdominal angiostrongyliasis in mice after worm maturation: preliminary trials. Jap. ,1. Parasit., 41: 481-486, 1992.
17. TUNGTRONGCHITR, A.; ISHII, A. & TERADA, M. - Effects of mebendazole given intermittently or successively with various doses and intervals on murine Angiostrongyliasis costaricensis after worm maturation. Jap. J. Parasit., 42: 321-330, I993a.
18. TUNGTRONGCHITR, A.; ISHII, A.; TERADA, M. & RADOMYOS, P. - Effects of sensitization on efficacy of mebendazole in mice infected with adult Angiostrongylus costaricensis. Trop. Mcd. Parasit., 44: 322-326, 1993b.
19. ZILIOTTO, A.; KUNZLE, J.E.; FERNANDES, L.A.R.; PRATES-CAMPOS, J.C. & BRITIO-COSTA, R. - Angiostrongilia.se: apresentacao de um provavel caso. Rev. Inst. Mcd. trop. S. Paulo, 17: 312-318, 1975.
Received: 30 October 2003
Accepted: 10 February 2004
Marcia Bohrer MENTZ(1), Carlos GRAEFF-TEIXEIRA(2) & Cinara Tcntardini GARRIDO(2)
Sponsorship from: PUCRS, FAPFRGS, CNPq. CAPES.
(1) Departamento de Microbiologia, Instituto de Ciencias Basicas da Saude da Universidade Federal do Rio Grande do SuI, RS, Brasil
(2) Faculdade de Biociencias da Pontificia Universidade Catolica de Porto Alegre, RS, Brasil
Correspondenee to: Marcia Bohrer Menlz. Run Fcrnandes Vieira 634, ap. 801, Bairro Born Firn, 90035-090 Porto Alegre. RS, Brasil, e- mail: mbmentz@uol.com.br
Copyright Instituto de Medicina Tropical de Sao Paulo Mar/Apr 2004
Provided by ProQuest Information and Learning Company. All rights Reserved