Rheumatoid arthritis
Rheumatoid arthritis (RA) is a chronic, inflammatory autoimmune disorder that causes the immune system to attack the joints. It is a disabling and painful inflammatory condition, which can lead to substantial loss of mobility due to pain and joint destruction. more...
The disease is also systemic in that it often also affects many extra-articular tissues throughout the body including the skin, blood vessels, heart, lungs, and muscles.
The name is derived from the Greek rheumatos meaning "flowing", the suffix -oid meaning "in the shape of", arthr meaning "joint" and the suffix -itis, a "condition involving inflammation".
Features
Rheumatoid arthritis is a chronic, inflammatory multisystem autoimmune disorder. It commonly affects the joints in a polyarticular manner (polyarthritis). The symptoms that distinguish rheumatoid arthritis from other forms of arthritis are inflammation and soft-tissue swelling of many joints at the same time (polyarthritis). The joints are generally affected in a symmetrical fashion. The pain generally improves with use of the affected joints, and there is usually stiffness of all joints in the morning that lasts over 1 hour. Thus, the pain of rheumatoid arthritis is usually worse in the morning compared to the classic pain of osteoarthritis where the pain worsens over the day as the joints are used.
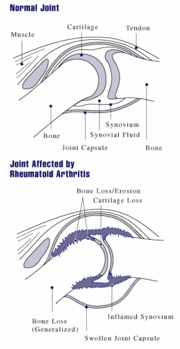
If the arthritis has been longstanding, the inflammatory activity has led to erosion and destruction of the joint surface, which impairs their range of movement and leads to deformity. The fingers are typically deviated towards the little finger (ulnar deviation) and can assume unnatural shapes. Classical deformities in Rheumatoid arthritis are the Boutonniere deformity (Hyperflexion at the proximal interphalangeal joint with hyperextension at the distal interphalangeal joint), Swan neck deformity (Hyperextension at the proximal interphalangeal joint, hyperflexion at the distal interphalangeal joint). The thumb may develop a "Z-Thumb" deformity with fixed flexion and subluxation at the metacarpophalangeal joint, leading to a "squared" appearance in the hand.
Subcutaneous nodules on extensor surfaces, such as the elbows, are often present.
Extra-articular manifestations also distinguish this disease from osteoarthritis (hence it is a multisystemic disease). Haematological: Most patients also suffer of anemia, either as a consequence of the disease itself (Anaemia of Chronic disease) or as a consequence of gastrointestinal bleeding as a side effect of drugs used in treatment, especially NSAIDs (non-steroidal anti-inflammatory drugs) used for analgesia. Splenomegaly may occur (Felty's syndrome).
Dermatological: Subcutaneous nodules
Pulmonary: The lungs may become involved as a part of the primary disease process or as a consequence of therapy. Fibrosis may occur spontaneously or as a consequence of therapy (for example methotrexate). Caplan's nodules are found as are pulmonary effusions.
Read more at Wikipedia.org