Crystal-induced synovial inflammation due to monosodium urate (MSU, gout) or calcium pyrophosphate dihydrate (CPPD, pseudogout) can cause acute arthritis among older patients. Gout and pseudogout may coexist with other joint diseases, and their diagnosis may be suggested by comorbid medical conditions (eg, hypothyroidism may indicate the presence of CPPD, renal insufficiency may indicate the presence of MSU) or drug therapies (eg, some diuretics can cause hyperuricemia). Although typically presenting as acute and self-limited attacks of mono- (single joint) or oligo- (<5 joints) arthritis, both may be polyarticular and chronic.
Crystal arthritis should be considered in the differential diagnosis of polyarthropathy, sometimes mimicking osteo- and rheumatoid arthritis. Acute gouty episodes affect peripheral joints (feet, hands) and last 3 to 10 days, whereas pseudogout more commonly involves intermediate joints (knees, wrists) and has a more prolonged course.
The expression of each is a function of systemic (age, race, sex, genetic factors, other metabolic disorders) and joint-specific (structure, function, tissue damage, ischemia, local temperature, pH) factors. At approximately 40 [micro]m (though varying considerably in configuration and size), MSU and CPPD crystals are readily visualized microscopically in neat or centrifuged joint fluid. They can be distinguished by compensated polarizing microscopy, which reveals differences in shape (rhomboid with blunt ends for CPPD, needle-shaped for MSU) and birefringence (strong and negative for MSU, weak and positive for CPPD) (figure).
[FIGURE OMITTED]
Gout
In older patients, gout is particularly challenging, because it can present atypically, and because treatment options are limited compared to the younger adult. (1)
Prevalence of gout is approximately 8.4 per 1,000 persons, and is 6 times more common in men than women. (2) Gout is rare in women before menopause, and the majority of young and middle-aged persons affected by this disease are men. The increasing prevalence in this group may relate to the overall incidence of obesity, hypertension, specific dietary habits and alcohol consumption, and the insulin resistance syndrome.
In the geriatric population, gout becomes a disease predominantly affecting women. Growing prevalence among older women may reflect increased longevity; improved survival of patients with diabetes, atherosclerosis, and heart failure; and the greater use of thiazide diuretics and aspirin prophylaxis for hypertension and heart disease.
More than 85% of women who develop gout have onset after menopause. After age 60, 50% to 60% of new patients established to have gout are women. (1,3,4) After age 80, virtually all new cases of gout are women. In this population, arthritis is more often polyarticular at onset, and there is a lower incidence of podagra, ie, pain and swelling of the big toe. "Impostumous" is a term used to describe tophaceous gout developing in Heberden's or Bouchard's nodes of older women with osteoarthritis. (5) Overall, more than 75% of gout diagnoses in geriatric patients are associated with diuretic use; alcohol is less often a cause.
Clinical presentation
Podagra. Severe pain and swelling in the first metatarsophalangeal joint (podagra) is the presenting feature in approximately 50% of gouty patients, and eventually develops in approximately 80%. Other affected joints include the ankles, tarsal and other metatarsal joints, knees, and elbows. Unlike pseudogout, the shoulder is rarely involved.
Following the first attack of gout, approximately 66% of patients will experience a second attack within 1year; 16% will experience a second attack within 1 to 2 years; 6% will experience the second attack 2 to 3 years later; and 5% will not experience a second attack for 3 to 5 years. Once established, without treatment, attacks become more frequent. (6)
Chronic tophaceous gout. This form of gout is characterized by polyarticular disease, no intercritical periods, and the development of masses of urate crystals in cartilage (which may be visualized at arthroscopy), and synovium/tendons/bone, which may be delineated by magnetic resonance imaging (MRI) or ultrasound. (7) An examination for tophi should include the olecranon bursa of the elbow, and the helices of the ear. This stage may take approximately 12 years to develop in idiopathic gout, with a faster time course in settings where there is an increased incidence of gout, such as organ transplantation patients on cyclosporine.
To further complicate diagnosis, uric acid levels in chronic tophaceous gout may be normal, even though the total miscible pool is increased. Chronic tophaceous gout, particularly involving the pulps of the fingers, may be the presentation of gout in older persons. (6)
Pathophysiology
Normal human serum urate levels are 2 to 8 mg/100 mL. The theoretical limit for urate solubility is approximately 7mg/100ml at 37[degrees]C. (8)
Hyperuricemia may be due to dietary excess (exogenous pathway), overproduction of urate due to cell turnover (endogenous pathway), or inefficient excretion (renal pathway). As the uric acid level increases above 9 mg/dL, the annual incidence of gouty arthritis increases; above 10mg/dL, the 5-year prevalence is 30%. (9)
Gout may be primary or associated with other diseases. Most patients with primary gout are inefficient excretors; 10% to 25% are overproducers.
Secondary causes of inefficient excretion are renal failure and diuretic therapy. Myeloproliferative diseases, and occasionally severe psoriasis, can lead to secondary gout caused by overproduction. In the insulin resistance syndrome--which is associated with glucose intolerance, visceral obesity, hypertension, dyslipidemia, and an increased incidence of arteriosclerotic heart disease and arterial thrombosis--hyperuricemia and nephrolithiasis may be a consequence of hyperinsulinemia directly stimulating urate reabsorption, and increasing urinary acidity due to an induced defect in renal ammonium excretion.10 In older patients, pathogenic factors to consider are decreased creatinine clearance, diuretics (furosemide/hydrochlorothiazides), and aspirin. (1,11,12)
Recent prospective studies have shown that the risk of gout is significantly increased with the ingestion of purine-rich foods, notably including red meats (RR 1.41 in the quintile with the highest intake compared to the quintile with the lowest intake) and seafood (RR 1.51). Of interest is an old observation that a low-dairy diet may decrease (RR 0.56) the incidence of gout. (13)
Among alcoholic beverages, the highest risk (2.51) was associated with imbibing 2 or more 12-oz beers per day, whereas alcoholic spirit beverages and wine (1 to 2 glasses per day) had lesser effects (RR 1.15 and 1.04, respectively).14
Diagnosis
An elevated uric acid level does not necessarily confirm the diagnosis of gout, although the incidence of gout and uric acid nephropathy (urolithiasis and interstitial nephropathy), increases with uric acid >9 mg/100 mL. (9) Excretion of uric acid may be monitored by a 24-hour collection or by calculation of urate/creatinine ratio on a spot urine using an algorithm normalized for glomerular filtration rate. (15) A diagnosis of gout confers a relative risk (2.2) of developing kidney stones, although the development of kidney stones does not increase the risk of developing gout. Gout may also increase the risk of calcium oxalate (the most common form) stone formation, possibly due to low urine pH consequent to defective renal production of ammonia.
Imaging of the affected joints can be helpful for diagnosis and in guiding long-term therapy. Erosive changes tend to be periarticular and have "overhanging edges" with preservation of the joint space. Areas such as the spinal column might be difficult to evaluate with plain radiographs; in such patients, MRI may be helpful. The definitive diagnosis of crystal arthropathy is made by arthrocentesis and analysis with a polarizing microscope. (16)
Pseudogout
Pseudogout (also known as calcium pyrophosphatate dihydrate deposition disease) was first recognized in 1961 as a mono- or oligoarticular disease resembling gout that was acute, accompanied by striking inflammation, and self-limited. The knee is most commonly affected, followed by the wrist, shoulder, and ankle.
Clinical presentation
Presentations of pseudogout may resemble rheumatoid arthritis, ankylosing spondylitis, hemarthrosis, and neuropathic arthropathy. There is an intimate relationship with osteoarthropathy, as pseudogout is an important diagnostic consideration in the evaluation of degenerative arthritis with an unusual distribution.
Pseudogout may be primary (sporadic), familial, or secondary to a number of metabolic diseases, including hemochromatosis, Wilson's disease, hyperparathyroidism, hypothyroidism, and hypomagnesemia; in a small number of patients, gout and pseudogout may coexist. Pseudogout in older persons is almost always sporadic, and may be acute (average age approximately 65; equal male and female occurrence) or chronic (average age 75; F>M). (11,12)
Pathophysiology
Calcium pyrophosphate crystals form as a consequence of elevated local levels of calcium and pyrophosphate (PPi). The latter, like uric acid, is a normal metabolite, resulting from the conversion of adenosine triphosphate (ATP) to adenosine monophosphate (AMP). Conditions associated with increased activity of ATP pyrophosphohydrolase and cyclic AMP may result in elevated PPi. The chondrocyte lacuna in cartilage is an important locus for PPi accumulation and crystal formation. This appears to be an age-related phenomenon, as Transforming growth factor beta-1 (TGFb1) increases PPi levels to a greater extent in chondrocytes from older persons. (17)
Diagnosis
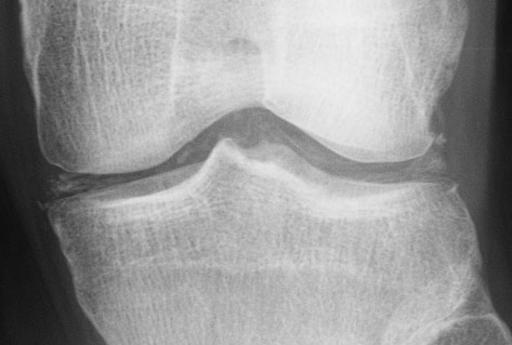
The diagnosis of pseudogout may be based on the clinical presentation, pattern of joint involvement (more commonly involving the wrist, knee, or shoulder) and radiographic intra-articular calcifications (chondrocalcinosis). Chondrocalcinosis may be asymptomatic, or associated with clinical pseudogout. Sites of predilection are the hyaline and fibrocartilage of the knee, the triangular ligament of the wrist, symphysis pubis, and hyaline cartilage of the hips and shoulders.
Chondrocalcinosis is an age-related phenomenon, increasing from 10% to 15% in adults age 65 to 75 to >40% in persons age 80 and older, and is often associated with osteoarthritis. (11,12) Other radiographic features suggestive of pseudogout include calcification of periarticular structures (tendon insertions, joint capsule, bursae), and isolated involvement of the patellofemoral, radiocarpal, or talocalcaneonavicular articulations. (18)
Definitive diagnosis requires identification of crystals in joint fluid. Because of weak birefringence, and often smaller size, accurate diagnosis can be more subtle than for gout, and may require comparison of spun synovial fluid by light and polarizing microscopy, and the examination of multiple fields. (16)
Treatment
The initial goal of therapy for crystal arthropathy is to terminate acute symptoms, and the long-term goal is to blunt future attacks and prevent erosive disease.
Management of acute gout/pseudogout
Options for treatment of acute attacks include colchicine, non-steroidal anti-inflammatory drugs (NSAIDS), and corticosteroids (table 1). Use of any of these medications in the geriatric population needs to be carefully considered with regard to reduced baseline creatinine clearance, the potential for NSAID gastropathy, fluid retention, and hypertension, and interactions with concomitant medications, such as warfarin.
When used in appropriate doses (0.6 mg/tid-qid), and early in an attack, colchicine blunts the inflammatory response, and may dramatically reduce pain and swelling; it is less effective for chronic tophaceous disease.
Selective cyclooxygenase-2 (COX-2) inhibitors have a lower incidence of GI events and are probably safer than other NSAIDS in older adults. However, these agents still may cause edema and hypertension, and can interfere with renal function. COX-2 inhibitors should be used with caution and only for short periods of time (ie, weeks, not months). (19)
Corticosteroids are a useful treatment option in older patients. They are as effective as NSAIDs, and may be used when NSAIDs are contraindicated or ineffective. Steroids can be given intra-articularly, intramuscularly, intravenously, or orally, depending on the number of involved joints, extent of systemic inflammation, and constitutional symptoms.
In monoarticular arthritis, intra-articular steroid injection is most effective and best-tolerated. Prior to injection, aspirate the affected joint and remove as much fluid as possible. This will provide symptomatic relief, confirm the diagnosis, and rule out co-existent septic arthritis. (20) Fluid should be sent for crystal analysis, cell count, gram stain and culture. If crystals are present and the gram stain is negative, it is safe to inject 5 to 10 mg of either triamcinolone or methylprednisolone into the small joints of the hands and feet, and 40 to 80 mg into larger joints, such as the knees. (21)
Polyarticular attacks respond well to systemic steroids. In older patients, a short course of corticosteroids is effective and well-tolerated. Systemic infections, such as endocarditis, may also cause polyarticular arthritis. Therefore, it is advisable to aspirate, examine, and culture fluid from an affected joints, as in monoarticular arthritis, and to send more than two sets of blood cultures for laboratory testing.
Early and mild polyarticular attacks can be aborted with a single dose of intramuscular triamcinolone or methylprednisolone, 40 to 80 mg. Severe attacks require a course of oral prednisone, 40 to 60 mg/d and tapered as symptoms permit, or intravenous steroids at an equivalent dose. (4,8)
Management of chronic gout/pseudogout Patients experiencing a single episode do not require long-term treatment. Following diagnosis, a concerted effort should be made to identify precipitating factors and metabolic abnormalities (eg, diet and alcohol for gout, hyperparathyroidism for pseudogout). However, treatment of associated metabolic diseases generally has little effect on the course of pyrophosphate arthropathy. Patients should be counseled to modify any behavioral factors and taught to recognize the early signs of an attack. The physician should be aware also that compliance may be a management issue, due to lack of willingness to adjust lifestyle, seek follow-up, or pursue chronic treatment. (22)
Metabolic approaches to the treatment of hyperuricemia and gout include reducing dietary purines and alcohol intake and managing obesity. Low-purine diets are difficult to adhere to, and may only reduce serum uric acid by approximately 15%. The ability of low-carbohydrate diets--in which meat ingestion is encouraged (eg, Atkins)--to increase serum uric acid is untested; however, a modified low-carbohydrate diet tailored to patients with insulin resistance was able to lower urate levels by approximately 18%. (23)
Recurrent (ie, more than 3 times per year) attacks of gout, urate nephropathy, tophi, or erosive changes on radiograph, are all indications for uric acid-lowering therapy (table 2). Current options include the uricosuric agents, probenecid and sulfinpyrazone, and the xanthine oxidase inhibitor, allopurinol.
Patients with a creatinine clearance greater than 50 mL per minute and, who excrete less than 700 mg of urinary uric acid per 24 hours, are candidates for uricosuric therapy with probenecid or sulfinpyrazone. These agents block tubular resorption of uric acid and have the potential to precipitate renal stones; a history of nephrolithiasis precludes their use. Uricosurics have a limited role in the treatment of patients over age 70. Patients on these treatments should have their urine alkalinized with bicarbonate to prevent renal stones. (1,4,8)
Long-term management
Long-term management of patients with gout includes adjustment of medications contributing to hyperuricemia. In patients with congestive heart failure (CHF) or hypertension who require high doses of diuretics, maximizing other modalities may decrease the need for diuresis and hence the frequency of gouty attacks. The angiotensin II receptor antagonist losartan, 100 mg/d, has a mild uricosuric effect, and is an adjunctive therapeutic option in older patients with either CHF or hypertension. The lipid-lowering agent, fenofibrate, 200 mg/d, also has a modest uricosuric effect. (24)
The xanthine oxidase inibitor allopurinol, the only one currently approved for use in the United States, is generally well-tolerated and effective both for patients who inefficiently excrete, or for those who overproduce, uric acid. The typical dose required to achieve an adequate response is 300 mg/d. Allopurinol may be associated with a number of significant adverse effects, including hepatotoxicity and hypersensitivity syndromes (2% to 4%); the latter (skin rashes, fever, hematologic abnormalities, nephritis) correlate with decreased renal function or the concomitant use of thiazide diuretics and, in the severest form (Stevens-Johnson syndrome), have an approximate 30% mortality rate. Allopurinol should be used with caution in patients with hepatic impairment, and should be avoided in patients with previous hypersensitivity. Azathioprine severely inhibits its metabolism, and should not be given concomitantly.
Abrupt changes in serum uric acid levels can precipitate a gouty attack. Therefore, prior to initiating chronic therapy it is important to ensure that arthropathy is optimally controlled. Prophylactic colchicine, 0.6 mg/d, in patients with a creatinine clearance greater than 50 mL, or every other day in patients with creatinine clearance between 20 mL and 50 mL, is an adjunctive therapy when starting uric acid-lowering therapy. Patients with renal failure (creatinine clearance less than 20 mL) should be placed on low doses of allopurinol, 100 mg QD or QOD, with prednisone, 5 mg/d, for temporary prophylaxis.
Conclusion
Gout and pseudogout can be painful and debilitating conditions that rob older patients of their quality of life. It is imperative that primary care physicians treat, manage, and prevent these attacks. Laboratory tests and imaging studies are useful for making the diagnosis. Colchicine, NSAIDs, and corticosteroids can be prescribed for acute episodes, whereas lifestyle changes, uricosuric agents, and xanthine oxidase inhibitors are used to manage and treat chronic cases.
References
(1.) F am AG. Gout in the elderly. Clinical presentation and treatment. Drugs Aging 1998; 13(3):229-43.
(2.) Lawrence RC, Helmick CG, Arnett FC, et al. Estimates of the prevalence of arthritis and selected musculoskeletal disorders in the United States. Arthritis Rheum 1998; 41(5):778-99.
(3.) Arromdee E, Michet CJ, Crowson CS, O'Fallon WM, Gabriel SE. Epidemiology of gout: Is the incidence rising? J Rheumatol 2002; 29(11):2403-6.
(4.) Kim KY, Ralph Schumacher H, Hunsche E, Wertheimer Al, Kong SX. A literature review of the epidemiology and treatment of acute gout. Clin Ther 2003; 25(6):1593-617.
(5.) Fam AG, Stein J, Rubenstein J. Gouty arthritis in nodal osteoarthritis. J Rheumatol 1996; 23(14):684-9.
(6.) Yu TF. Diversity of clinical features in gouty arthritis. Semin Arthritis Rheum 1984; 13(4):360-8.
(7.) Gentili A. Advanced imaging of gout. Semin Musculoskelet Radiol 2003; 7(3):165-74.
(8.) Terkeltaub RA. Clinical practice. Gout. N Engl J Med 2003; 349(17):1647-55.
(9.) Kramer HJ, Choi HK, Atkinson K, Stampfer M, Curhan GC. The association between gout and nephrolithiasis in men: The Health Professionals' Follow-up Study. Kidney Int 2003; 64(13):1022-6.
(10.) Abate N, Chandalia M, Cabo-Chan AV Jr, Moe OW, Sakhaee K. The metabolic syndrome and uric acid nephrolithiasis: Novel features of renal manifestation of insulin resistance. Kidney Int 2004; 65(2):386-92.
(11.) Doherty M, Dieppe P. Crystal deposition disease in the elderly. Clin Rheum Dis 1986; 12(1):97-116.
(12.) Agudelo CA, Wise CM. Crystal-associated arthritis in the elderly. Rheum Dis Clin N Am 2000; 26(3):527-46.
(13.) Choi HK, Atkinson K, Karlson EW, Willett W, Curhan G. Purine-rich foods, dairy and protein intake, and the risk of gout in men. N Engl J Med 2004; 350(11):1093-103.
(14.) Choi HK, Atkinson K, Karlson EW, Willett W, Curhan G. Alcohol intake and risk of incident gout in men; a prospective study. Lancet 2004; 363(9417):1277-81.
(15.) Simkin PA. When, why, and how should we quantify the excretion rate of urinary uric acid? J Rheumatol 2001; 28(6):1207-10.
(16.) Dieppe P, Swan A. Identification of crystals in synovial fluid. Ann Rheum Dis 1999; 58(5):261-3.
(17.) Anderson HC. Matrix vesicles and calcification. Curr Rheumatol Rep 2003; 5(3):222-6.
(18.) Steinbach LS. Calcium pyrophosphate dihydrate and calcium hydroxyapatite crystal deposition diseases: Imaging perspectives. Radiol Clin North Am 2004; 42(1):185-205.
(19.) Schumacher, HR Jr, Boice JA, Daikh DI, et al. Randomized double blind trial of etoricoxib and indomethacin in treatment of acute gouty arthritis. BMJ 2002; 324(7352):1488-92.
(20.) Yu KH, Luo SF, Liou LB, et al. Concomitant septic and gouty arthritis--an analysis of 30 cases. Rheumatology (Oxford) 2003; 42(19):1062-6.
(21.) Alloway JA, Moriarty MJ, Hoogland YT, Nashel DJ. Comparison of triamcinolone acetonide with indomethacin in the treatment of acute gouty arthritis. J Rheumatol 1993; 20(11):111-3.
(22.) de Klerk E, van der Heijde D, Landewe R, van der Tempel H, Urquhart J, van der Linden S. Patient compliance in rheumatoid arthritis, polymyalgia rheumatica, and gout. J Rheumatol 2003; 30(1):44-54.
(23.) Fam AG. Gout, diet, and the insulin resistance syndrome. J Rheumatol 2002; 29(7):1350-5.
(24.) Bardin T. Fenofibrate and losartan. Ann Rheum Dis 2003; 62(6):497-8.
Source: Created for Geriatrics by M Cassetta, DO, and PD Gorevic, MD.
CME Geriatrics Exam
Detach or photocopy this page, place an X in the boxes that correspond to your answers, fill in your name and address, and mail (see address below). Answers must be received by March 1, 2005. A score of at least 80% must be earned to receive CME credit.
Make check for $15 payable to The Page and William Black Post-Graduate School and mail it with this exam to Rae Ann Houghton, Geriatrics, 7500 Old Oak Blvd., Cleveland, Ohio 44130. When submitting more than one exam, attach a separate check for $15 to each exam. Documentation of earned credit and the correct answers will be mailed to you. Allow up to 12 weeks for notification.
Accreditation. This activity has been planned and implemented in accordance with the Essentials and Standards of the Accreditation Council for Continuing Medical Education (ACCME) through the sponsorship of Mount Sinai School of Medicine. Mount Sinai School of Medicine is accredited by ACCME to provide continuing medical education for physicians. Mount Sinai School of Medicine designates this continuing medical education activity for a maximum of 1 credit in category 1 toward the AMA Physician's Recognition Award. Each physician should claim only those hours that he/she spent in the educational activity.
Faculty Disclosure. It is the policy of Mount Sinai School of Medicine to ensure fair balance, independence, objectivity, and scientific rigor in all its sponsored programs. All faculty participating in sponsored programs are expected to disclose to the audience any real or apparent conflict-of-interest related to the content of their presentation, and any discussions of unlabeled or investigational use of any commercial product or device not yet approved in the United States.
Take Home
* Crystal-induced arthritis in older adults may be acute, monoarticular, and self-limited, or chronic and polyarticular * Diagnosis may be suggested by signs of intense inflammation (rubor, calor) in the affected joint(s)
* Diagnosis may be suggested by which joints are inflamed, by characteristic x-ray findings, or by the presence of an associated disease
* Hyperuricemia is associated with diuretic use or renal insufficiency, both of which are significant risk factors in geriatric patients
* Although they may suggest the diagnosis of gout or pseudogout respectively, hyperuricemia or chondrocalcinosis may occur without the development of crystal-induced arthritis
* Comorbid medical conditions should be carefully considered with regard to precipitating factors, underlying diseases, and therapeutic strategies
* Treatment involves the relief of pain, swelling, and systemic inflammation that are typical of the acute attack, and the development of maintenance therapy in patients with frequently recurring or chronic symptoms
Source: Created for Geriatrics by M Cassetta, DO, and PD Gorevic, MD.
Dr. Cassetta is a fellow in rheumatology, Mount Sinai Medical Center, New York, NY.
Dr. Gorevic is professor of medicine and director of rheumatology, Mount Sinai Medical Center, New York, NY.
Disclosures: The authors have no real or apparent conflict of interest due to affiliation with any company or manufacturer whose products or devices are mentioned in this article.
COPYRIGHT 2004 Advanstar Communications, Inc.
COPYRIGHT 2005 Gale Group