The place of compartmental arthroplasty of the knee remains controversial. There has been a recent resurgence of interest after the publication of reports of longer-term survivorship from Europe, Scandinavia and the UK.1-3 In the 1960s and 1970s total knee replacement (TKR) achieved inconsistent results. In appropriate cases compartmental arthroplasty, a less invasive procedure, was capable of producing an outcome which was as good or better than that of total replacement. Over the last 25 years, however, there have been considerable improvements in the results from TKR. In the last two decades, various designs of implant have been shown to give excellent results equivalent to those of total hip arthroplasty.4,5 Consequently, many surgeons, particularly from North America, have questioned the need for compartmental arthroplasty. Although the long-term reviews of TKR show very satisfactory results, there continue to be a small number of patients with major complications in the short and medium term. Others suffer unexplained pain with functional results which are unsatisfactory. Together, these amount to between 10% and 20% of the total number of cases.3,5-7
Certain designs of unicompartmental arthroplasty continue to perform well and some centres in Europe, Scandinavia and the UK have continued to advocate their use in appropriate cases.1,2,3,8 This brief review describes the underlying pathology and indications for the procedure and draws attention to those reports in the literature which suggest a place for the continued use of this type of prosthesis.
Pathology
Epidemiological studies of osteoarthritis of the knee have shown that there are distinct patterns of disease which affect principally either the medial, lateral or patellofemoral compartments.9,10 Although there is some overlap between the different compartments, the speed of progression is usually very slow and the process can be confined to one part of the knee for many years. The medial compartment is most commonly affected. At least 25% of patients with osteoarthritis of the knee suffer from isolated medial compartment disease. The patellofemoral compartment is the next most frequently affected with isolated disease in up to 10% of patients. Changes restricted to the lateral compartment are less common and occur in less than 5% of cases. The biomechanical characteristics of the three main compartments of the knee are entirely different. The design criteria for the different compartments will therefore be quite different and the results to date of arthroplasty of the lateral compartment using a standard prosthesis have proved to be disappointing.11 In the last ten years better understanding of patellofemoral mechanics has improved this aspect of total knee arthroplasty and current designs of isolated patellofemoral arthroplasty may produce better results than in the past.12 This article will consider only osteoarthritis of the medial compartment.
The degenerative process usually starts in the anterior half of the tibial plateau and in the corresponding part of the medial femoral condyle when the knee is in 20[degrees] to 30[degrees] of flexion. This anteromedial disease13 is ideally suited to medial compartment arthroplasty. More extensive studies of pathological specimens in patients with intact, frayed and ruptured anterior cruciate ligaments (ACLs) have demonstrated a progression whereby the deepest point of wear moves posteriorly14 as the area of wear expands in the same direction (Fig. 1). Osteophytes develop in the intercondylar notch as the process proceeds and attrition and final rupture of the ACL causes intercondylar impingement and lateral subluxation of the tibia, the effect of which can be seen on plain radiographs. Initially, the varus deformity of the joint corrects to neutral, but as the process progresses a fixed deformity develops in conjunction with rupture of the ACL. Rupture of the ACL produces a loss of anteroposterior stability which prevents the proper functioning of a medial compartment arthroplasty.15
Investigations
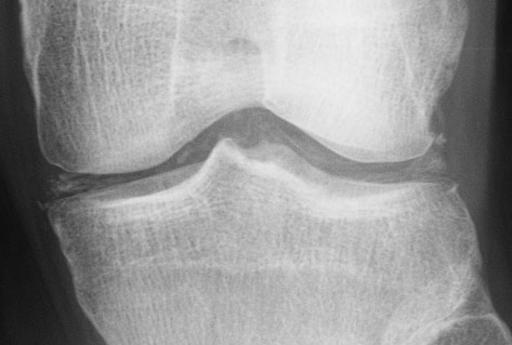
The standard investigations should always include weight-bearing films. The anteroposterior view should be taken in full extension and repeated at 20[degrees] of flexion, the so-called schuss view. This will demonstrate the narrowest part of the joint space. The standing lateral view should also be taken at 20[degrees] of flexion. This will show the outlines of the medial and lateral compartments and the position of wear on the tibial plateau (Fig. 2). Wear of the posterior plateau always reflects attrition or rupture of the ACL indicating the unsuitability for compartmental arthroplasty. A tangential view of the patellofemoral joint should be taken at 30[degrees] of flexion (Merchant's view) to exclude patellofemoral disease. There is a significant subgroup, which shows arthritic change in the medial tibiofemoral compartment and in the medial facet of the patella. Although correction of the varus will unload the medial facet, more advanced changes will be a contraindication to isolated medial arthroplasty.
Radiological investigations with long standing views and strain views can be helpful, but seldom add significant information. The use of MRI can give further information about the articular cartilage and soft-tissue structures. Degenerative changes are often seen in the cruciate ligaments but MR scans are too sensitive to give any useful information about the function of the ACL.16
Arthroscopic assessment of the knee may be useful in some cases. Younger patients with early disease can achieve symptomatic benefit from meniscal trimming, chondrectomy, microfracture and generalised lavage. In established cases plain weight-bearing radiographs will generally give an accurate assessment of the pathology in order to allow a decision to be made on the type of arthroplasty.
Indications
The long-term success of medial unicompartmental arthroplasty depends on choosing appropriate cases. Robertsson et al17 have shown convincingly that experience is an important factor in achieving satisfactory long-term results. They found that those centres performing more than 23 cases per year were able to achieve better results with the Oxford and St Georg Sled arthroplasties than those undertaking fewer numbers. They also showed that experience did not improve the results of an unsatisfactory prosthesis. The authors considered that an important factor for success was a proper understanding of the philosophy involved in unicompartmental arthroplasty, which enabled a particular centre to choose more appropriate cases. A degree of judgement is required in both choosing the cases and undertaking the procedure and this is something which cannot be taught easily, and is acquired only with experience.
First, an accurate and detailed diagnosis is necessary. There should be relatively early isolated medial compartment disease with an intact ACL, a correctable varus deformity with no significant fixed flexion and a good passive range of movement. In addition, the lateral compartment should be normal and there should be only minor damage to the patellofemoral joint. Chondrocalcinosis is not a specific contraindication. In many cases the disease will have been active for a number of years and all the articular surfaces will have been exposed to the adverse effects of inflammatory synovial fluid. Studies on the apparently normal lateral compartment have shown reduced mechanical strength emphasising the importance of slightly undercorrecting the overall alignment.18
Patients suffering from an inflammatory polyarthropathy should not be considered for compartmental arthroplasty even when there appears to be end-stage medial osteoarthritis. As to the patellofemoral joint, it is a question of judgement as to how much damage to the articular surfaces can be accepted before deciding to proceed with unicompartmental arthroplasty.
The age of the patient can raise different philosophical arguments. Compartmental arthroplasty may not be appropriate in young and active patients, in whom osteotomy is the treatment of choice. There have been few studies which have reviewed younger patients after knee replacement. Case, Ackroyd and Newman19 described the outcome after six years in patients under the age of 60 years and found no difference between the Kinematic total knee and the medial St Georg Sled arthroplasties. The clinical results were slightly worse in both groups than the mean results for all ages. The weight of the patient and the body mass index have been considered to be criteria in the selection of patients although this has never been clearly defined. It is probably inadvisable to use this type of arthroplasty in active heavily-built patients, particularly those with a large medial gait moment.
In centres which regularly perform unicompartmental arthroplasty about 20% of patients with painful medial compartment osteoarthritis will be eligible for this procedure. In order to achieve success it is necessary to understand the underlying pathological condition, to be fully familiar with the technical procedure and to be able to deal successfully with any complications which may arise.
Prosthesis and Technique
There have been many designs of unicompartmental replacement but few have achieved acceptable long-term survivorship.1-3,17,20 A number of new prostheses have been introduced in the last five years but there are no long-term results available and no evidence to suggest that they will be more successful than the existing designs which have been used for 30 years. The concept of a compartment replacement relies on the preservation of intact ligaments. It is therefore essential that the prosthesis be totally unconstrained. This can be achieved in two ways. First, a biconvex femoral component articulating with a totally flat plateau can be used (Fig. 3). This inevitably means that initially there is a non-congruous articulation, which will lead to high loading on the polyethylene and, in theory, early failure. Two prostheses of this design, the Marmor and St Georg Sled, have produced successful clinical results.3,21 The wear rate for the St Georg Sled is 0.08 mm per year, which is considerably lower than might be expected.22 It has been suggested that creep of the polyethylene in the first few years produces an optimally placed indentation which will then reduce the loading on the polyethylene. There may also be hardening of the material in the area of the indentation. The all-polyethylene tibial component may allow some absorption of the cement bone forces. Loosening of the tibial component is seldom seen in the absence of major ligamentous or structural failure.
The second method of achieving an unconstrained prosthesis is by the use of a mobile meniscal bearing (Fig. 4). This design was pioneered by Goodfellow and O'Connor23 with the Oxford prosthesis, which has achieved excellent results in some centres.1,2 There is a fully congruent bearing of the meniscofemoral articulation, which is maintained throughout the full range of movement. Unconstrained movement of the meniscus occurs on the flat tibial surface. This design allows near to normal knee kinematics and minimises polyethylene wear to less than 0.036 mm per year.24 However, dislocation of the bearing can occur if perfect balancing of the ligaments in both flexion and extension is not achieved.
There are a number of designs which combine elements of these two opposing principles but none has yet produced convincing long-term success.
The fixed-bearing prosthesis is technically straightforward and can be performed satisfactorily with relatively little experience. A disadvantage is that there is a higher rate of wear which will begin to have its effect in the second decade of use. The mobile bearing, by contrast, is technically more difficult to perform and some centres have not been able to achieve consistent results. If performed frequently with technical accuracy, experienced surgeons can achieve excellent results with a low potential for wear in the second or even the third decades.2 Those undertaking small numbers of operations each year are best advised to avoid a technically demanding design. Training courses and dry bone workshops are invaluable in achieving technical competence.
A major advantage of a unicompartmental arthroplasty is that it can be performed through a relatively small incision which need not be extended into the quadriceps tendon. The patella can be subluxed laterally to provide adequate exposure of the medial femoral condyle. A subvastus extension of the retinacular incision will allow excellent access to the posterior part of the joint which is essential in order to remove residual fragments of cement from the posterior edge of both the tibial and femoral components. A minimally invasive exposure is being pioneered in some centres and this can reduce the hospital stay to less than 24 hours.25 In these cases considerable experience is required to achieve satisfactory implantation.
Results
The Swedish Knee Registry26 has documented many thousands of joint replacements and each year their annual report published on the Internet shows the up-to-date survivorship of different prostheses. The results are pooled from all contributing centres and are thus likely to give a reasonable assessment of the overall outcome. Reports from single authors or centres tend to give an optimistic assessment of the results of a particular prosthesis showing the best that can be achieved in the most expert hands. The results from the Knee Registry for 2001 show that the St Georg Sled is achieving a cumulative revision rate of 5% at nine years, which is similar to the results of a standard TKR. The Oxford arthroplasty, by contrast, records an overall cumulative revision rate of 14% at nine years. Some centres are achieving much better results than others. Svard and Price,2 in a large single-centre study achieved a survivorship rate of 95% at ten years and 94% at 15 years. This is slightly worse than the 98% reported by Murray et al1 from a smaller single-surgeon series.
When all the prostheses and centres are taken together it is clear that TKR has improved considerably over the last 20 years. Most centres are able to obtain similar results with a variety of prostheses with a cumulative revision rate of 5% to 10%. When all reviews of unicompartmental prostheses are considered the results have not improved over the last 20 years. However, certain prostheses can achieve consistently good results in all centres and the analysis of Robertsson et al17 of more than 12 000 compartmental arthroplasties performed between 1986 and 1995 examined the various factors which determine success.
The Bristol Knee Group8 have shown comparable survivorship at five years in a randomised controlled trial of the Kinematic TKR and the St Georg Sled. A larger ten-year survivorship study of these two prostheses performed in Bristol, a standard National Health Service clinic with many operations being performed by surgeons in training, showed no significant difference between the two prostheses both for survivorship and for significant pain (Fig. 5).
The principal arguments in favour of unicompartmental arthroplasty are that the procedure is much less invasive than TKR, preserving the undamaged soft tissue and articular structures and restoring the joint to more normal function. The speed of recovery is considerably faster, particularly when a reduced or minimally invasive approach is used. Complications such as infection, thromboembolic episodes and stiffness of the joint are reduced considerably.8,27
Failure of a unicompartmental arthroplasty requires revision to TKR. It may occur as a result of inappropriate patient selection, poor soft-tissue balancing or malposition of the components. The mobile-bearing prostheses may be more sensitive to malposition of the components than a fixed-bearing implant with an all-polyethylene tibia. Late failure may occur from progression of the disease in one of the other compartments of the joint, although follow-up studies have shown that the rate of deterioration is extremely slow.21,28,29 Revision to TKR is generally straightforward. Bone defects occur infrequently and can easily be reconstructed by available bone graft or the use of modular prostheses. Revision is easier with an all-polyethylene tibia and Chakrabarty, Newman and Ackroyd30 reported that 80% of a group of revisions of the St Georg Sled were similar to primary knee replacement.
Summary
Compartmental arthritis forms a significant subgroup of patients presenting with osteoarthritis of the knee. Involvement of the medial compartment is the most common and can be successfully treated by unicompartmetal arthroplasty. The first step is to obtain an accurate diagnosis of the process of the disease, and, particularly, to evaluate the integrity of the ACL. Assessment requires clinical, radiographic and perhaps arthroscopic evaluation, but the final decision will depend upon judgement taken at the time of the arthrotomy. This improves with experience and it is essential that the surgeon has sufficient basic understanding and regular practice.
The decision on the design of the prosthesis is critical. This should be based on ten-year survivorship studies with a success rate of at least 85% to 90%. The technically more demanding prostheses can give excellent long-term results in some centres. The less complex prostheses can produce good long-term results in more general use.
Most studies consistently report lower complication rates, more rapid recovery and long-term results of better quality than TKR. Set against this must be the recognition that failure because of progression of the disease can occur in addition to that due to mechanical causes. There is no convincing evidence that the well-tried and tested prostheses have a significantly greater overall rate of failure than TKR.
Reports of revision show that this is not technically demanding and is considerably simpler than for failed TKR with results which are probably little different from those of a primary arthroplasty.
The resurgent interest in compartmental arthroplasty is based on encouraging reports from those few centres which have pioneered the treatment. Successful results require a detailed knowledge of the pathology, indications, technique and management of the procedure. This philosophy adds several extra dimensions to the routine of established knee arthroplasty.
References
1. Murray DW, Goodfellow JW, O'Connor JJ. The Oxford medial unicompartmental arthroplasty: a ten-year survival study. J Bone Joint Surg [Br] 1998;80-B:983-9.
2. Svard UCG, Price AJ. Oxford medial Unicompartmental knee arthroplasty: a survival anlaysis of an independent series. J Bone Joint Surg [Br] 2001;83-B:191-4.
3. Ackroyd CE, Whitehouse SL, Newman JH, Joslin CC. A comparative study of the medial St George Sled and Kinematic Total Knee arthroplasties: ten-year survivorship. J Bone Joint Surg [Br] 2002;84-B:667-72.
4. Gill GS, Joshi AB. Long-term results of kinematic condylar knee replacement: an analysis of 404 knees. J Bone Joint Surg [Br] 2001;83-B:355-8.
5. Ansari S, Ackroyd CE, Newman JH. Kinematic posterior cruciate ligament: retaining total knee replacements: a ten-year survivorship study of 445 arthroplasties. Am J Knee Surg 1998;11:9-14.
6. Ritter MA, Campbell E, Faris PM, Keating EM. Long-term survival analysis of the posterior cruciate condylar total knee arthroplasty: a ten-year evaluation. J Arthroplasty 1989;4:293-6.
7. Murray DW, Frost SJD. Pain in the assessment of total knee replacement. J Bone Joint Surg [Br] 1998;80-B:426-31.
8. Newman JH, Ackroyd CE, Shah NA. Unicompartmental or total knee replacement? Five year results of a prospective randomised trial of 102 osteoarthritic knees with unicompartmental arthritis. J Bone Joint Surg [Br] 1998;80-B:862-5.
9. McAlindon TE, Snow S, Cooper C, Dieppe PA. Radiographic pattern of osteoarthritis of the knee joint in the community: the importance of the patello-femoral joint. Ann Rheum Dis 1992;51:844-9.
10. Davies AP, Vince AS, Shepstone L, Donell ST, Glasgow MM. The radiologic prevalence of patellofemoral osteoarthritis. Clin Orthop 2002;402:206-12.
11. Ashraf T, Newman JH, Evans R, Ackroyd CE. Lateral unicompartmental knee arthroplasty. J Bone Joint Surg [Br] 2002;84-B:1126-30.
12. Ackroyd CE, Newman JH. The Avon patello-femoral arthroplasty: two to five year results. J Bone Joint Surg [Br] 2003;85-B:(Suppl II):162.
13. White SW, Ludkowski PF, Goodfellow JW. Anteriomedial osteoarthritis of the knee. J Bone Joint Surg [Br] 1991;73-B:582-6.
14. Porteous AJ, Ackroyd CE. Tibial topography in gonarthrosis. J Bone Joint Surg [Br] 2001;83-B(Suppl II):259.
15. Goodfellow J, O'Connor J. The anterior cruciate ligament in knee arthroplasty: a risk factor with unconstrained meniscal prosthesis. Clin Orthop 1992;276:245-52.
16. Sharp I, Tyrrell PNM, White SH. Magnetic resonance imaging assessment for unicompartmental knee replacement: a limited role. The Knee 2001;8:213-8.
17. Robertsson O, Knutson K, Lewold S, Lidgren L. The routine of surgical management reduces failure after unicompartmental knee arthroplasty. J Bone Joint Surg [Br] 2001;83-B:45-9.
18. Obeid EMH, Adam MA, Newman JH. Mechanical properties of articular cartilage in knees with unicompartmental osteoarthritis. J Bone Joint Surg [Br] 1994;76-B:315-9.
19. Case RD, Ackroyd CE, Newman JH. The outcome of knee replacement in patients under 60 years of age. J Bone Joint Surg [Br] 2001;83-B(Suppl II):244.
20. Lewold S, Robertsson O, Knutson K, Lidgren L. Revision of unicompartmental knee arthroplasty: outcome in 1135 cases from the Swedish Knee Arthroplasty study. Acta Orthop Scand 1998;69:469-74.
21. Squire MW, Callaghan JJ, Geoty DD, Sullivan PM, Johnston RC. Unicompartmental knee replacement: a minimum 15 year follow-up study. Clin Orthop 1999;367:61-72.
22. Desai V, Newman JH. Polyethylene wear in a non-congruous unicompartmental knee replacement: a retrieval analysis. Transactions of the IMechE Conference on Knee Replacement 1999; 1974-2024.
23. Goodfellow JW, O'Connor JJ. The mechanics of the knee and prosthesis design. J Bone Joint Surg [Br] 1978;60-B:358-69.
24. Psychoyios V, Crawford RM, O'Connor JJ. Wear of congruent meniscal bearings in unicompartmental knee arthroplasty: a retrieval study of 16 specimen. J Bone Joint Surg [Br] 1998;80-B:976-82.
25. Price AJ, Webb J, Topf H, et al. Rapid recovery after Oxford unicompartmental arthroplasty through a short incision. J Arthroplasty 2001;16:970-6.
26. Swedish Knee Arthropiasty Register. 2001: www.ort.lu.se/knee/indexeng
27. Ansari S, Warwick D, Ackroyd CE, Newman JH. Incidence of fatal pulmonary embolism after 1390 knee replacements without routine prophylaxis except in high risk cases. J Arthroplasty 1997;12:599-602.
28. Weale AE, Murray DW, Crawford R, et al. Does arthritis progress after medial unicompartmental knee replacement? J Bone Joint Surg [Br] 1999;81-B:783-9.
29. Weale AE, Murray DW, Baines J, Newman JH. Radiological changes five years after unicompartmental knee replacement. J Bone Joint Surg [Br] 2000;82-B:996-1000.
30. Chakrabarty G, Newman J, Ackroyd CE. Revision of unicompartmental arthroplasty: clinical and technical considerations. J Arthroplasty 1998;13:191-6.
C. E. Ackroyd
From the Avon Orthopaedic Centre, Bristol, England
C. E. Ackroyd, FRCS, Consultant Orthopaedic Surgeon
2 Clifton Park, Clifton, Bristol BS8 3BS, UK.
(C)2003 British Editorial Society of Bone and Joint Surgery
doi: 10.1302/0301-620X.85B7.14650 $2.00
J Bone Joint Surg [Br] 2003;85-B:937-42.
Copyright British Editorial Society of Bone & Joint Surgery Sep 2003
Provided by ProQuest Information and Learning Company. All rights Reserved