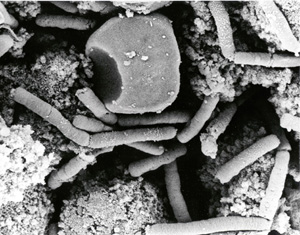
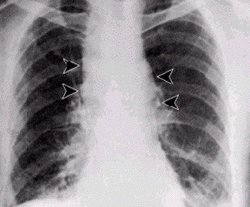
The Centers for Disease Control and Prevention (CDC) has issued an update on the investigation of recent cases of anthrax exposure. This update includes the susceptibility patterns of Bacillus anthracis isolates, and provides interim recommendations for managing potential threats and exposures and for treating anthrax. The complete report appears in the October 26, 2001 issue of Morbidity and Mortality Weekly Report and is available on the CDC Web site at www.cdc.gov/mmwr. A copy of the report is also available on the Web site of the American Academy of Family Physicians at www.aafp.org/resources.
Managing Exposure
The highest priority is to identify at-risk persons and initiate appropriate interventions to protect them. The exposure circumstances are the most important factors that direct decisions about prophylaxis. Persons with an exposure or contact with an environment known, or suspected, to be contaminated with B. anthracis--regardless of laboratory test results--should be offered antimicrobial prophylaxis. Exposure or contact, not laboratory results, is the basis for initiating treatment.
Antimicrobial Treatment
A high index of suspicion and rapid administration of effective antimicrobial therapy is essential for prompt diagnosis and effective treatment of anthrax. Limited clinical experience is available and no controlled trials in humans have been performed to validate current treatment recommendations for inhalational anthrax. Based on studies in nonhuman primates and other animals and in vitro data, ciprofloxacin or doxycycline should be used for initial intravenous therapy until antimicrobial susceptibility results are known (Table 1).
Two or more antimicrobial agents predicted to be effective are recommended because of the mortality associated with inhalational anthrax. Other agents with in vitro activity suggested for use in conjunction with ciprofloxacin or doxycycline include rifampin, vancomycin, imipenem, chloramphenicol, penicillin and ampicillin, clindamycin and clarithromycin, but other than for penicillin, limited or no data exist about using these agents in the treatment of inhalational B. anthracis infection. Cephalosporins and trimethoprim-sulfamethoxazole should not be used for therapy, and penicillin G and ampicillin alone should not be used to treat systemic infection because the combination may not be clinically effective for inhalational anthrax where large numbers of organisms are likely to be present.
Toxin-mediated morbidity is a major complication of systemic anthrax. Corticosteroids have been suggested as adjunct therapy for inhalational anthrax associated with extensive edema, respiratory compromise, and meningitis.
For cutaneous anthrax, ciprofloxacin and doxycycline are first-line therapy (Table 2). Intravenous therapy with a multidrug regimen is recommended if signs of systemic involvement, extensive edema, or lesions on the head and neck are present. Antimicrobial treatment may render lesions culture negative in 24 hours, but progression to eschar formation still occurs. Typically, cutaneous anthrax is treated for seven to 10 days, but with the latest attacks, the risk for simultaneous aerosol exposure appears to be high. Although infection may produce an effective immune response, a potential for reactivation of latent infection may exist, so patients should be treated for 60 days.
All medications may have side effects and allergic reactions. Physicians should be aware of these side effects and consult an infectious diseases specialist as needed. Patients should be urged to inform their health care provider of any adverse events.
COPYRIGHT 2001 American Academy of Family Physicians
COPYRIGHT 2002 Gale Group